* Served through May 2012.
† Served from June 2012 through October 2012.
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Please note: An erratum has been published for this article. To view the erratum, please click here.
Corresponding preparer: Amy Parker Fiebelkorn, MSN, Division of Viral Diseases, National Center for Immunization and Respiratory Diseases, CDC. Telephone: 404-639-8235; E-mail: aparker@cdc.gov.
Summary
This report is a compendium of all current recommendations for the prevention of measles, rubella, congenital rubella syndrome (CRS), and mumps. The report presents the recent revisions adopted by the Advisory Committee on Immunization Practices (ACIP) on October 24, 2012, and also summarizes all existing ACIP recommendations that have been published previously during 1998–2011 (CDC. Measles, mumps, and rubella—vaccine use and strategies for elimination of measles, rubella, and congenital rubella syndrome and control of mumps: recommendations of the Advisory Committee on Immunization Practices [ACIP]. MMWR 1998;47[No. RR-8]; CDC. Revised ACIP recommendation for avoiding pregnancy after receiving a rubella-containing vaccine. MMWR 2001;50:1117; CDC. Updated recommendations of the Advisory Committee on Immunization Practices [ACIP] for the control and elimination of mumps. MMWR 2006;55:629–30; and, CDC. Immunization of health-care personnel: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 2011;60[No. RR-7]).Currently, ACIP recommends 2 doses of MMR vaccine routinely for children with the first dose administered at age 12 through 15 months and the second dose administered at age 4 through 6 years before school entry. Two doses are recommended for adults at high risk for exposure and transmission (e.g., students attending colleges or other post-high school educational institutions, health-care personnel, and international travelers) and 1 dose for other adults aged ≥18 years. For prevention of rubella, 1 dose of MMR vaccine is recommended for persons aged ≥12 months.
At the October 24, 2012 meeting, ACIP adopted the following revisions, which are published here for the first time. These included:
As a compendium of all current recommendations for the prevention of measles, rubella, congenital rubella syndrome (CRS), and mumps, the information in this report is intended for use by clinicians as baseline guidance for scheduling of vaccinations for these conditions and considerations regarding vaccination of special populations. ACIP recommendations are reviewed periodically and are revised as indicated when new information becomes available.
Measles, rubella, and mumps are acute viral diseases that can cause serious disease and complications of disease but can be prevented with vaccination. Vaccines for prevention of measles, rubella, and mumps were licensed and recommended for use in the United States in the 1960s and 1970s. Because of successful vaccination programs, measles, rubella, congenital rubella syndrome (CRS), and mumps are now uncommon in the United States. However, recent outbreaks of measles (1) and mumps (2,3) have occurred from import-associated cases because these diseases are common in many other countries. Persons who are unvaccinated put themselves and others at risk for these diseases and related complications.
Two live attenuated vaccines are licensed and available in the United States to prevent measles, mumps, and rubella: MMR vaccine (measles, mumps, and rubella [M-M-R II, Merck & Co., Inc.]), which is indicated routinely for persons aged ≥12 months and infants aged ≥6 months who are traveling internationally and MMRV vaccine (measles, mumps, rubella, and varicella [ProQuad, Merck & Co., Inc.]) licensed for children aged 12 months through 12 years. For the purposes of this report, MMR vaccine will be used as a general term for measles, mumps, and rubella vaccination; however, age-appropriate use of either licensed vaccine formulation can be used to implement these vaccination recommendations.
For the prevention of measles, mumps, and rubella, vaccination is recommended for persons aged ≥12 months. For the prevention of measles and mumps, ACIP recommends 2 doses of MMR vaccine routinely for children with the first dose administered at age 12 through 15 months and the second dose administered at age 4 through 6 years before school entry. Two doses are recommended for adults at high risk for exposure and transmission (e.g., students attending colleges or other post-high school educational institutions, health-care personnel, and international travelers) and 1 dose for other adults aged ≥18 years. For prevention of rubella, 1 dose of MMR vaccine is recommended for persons aged ≥12 months. This report is a compendium of all current recommendations for the prevention of measles, rubella, congenital rubella syndrome (CRS), and mumps. The report presents the recent revisions adopted by the Advisory Committee on Immunization Practices (ACIP) on October 24, 2012, and also summarizes all existing ACIP recommendations that have been published previously during 1998–2011 (4–6). As a compendium of all current ACIP recommendations, the information in this report is intended for use by clinicians as guidance for scheduling of vaccinations for these conditions and considerations regarding vaccination of special populations.
Periodically, ACIP reviews available information to inform the development or revision of its vaccine recommendations. In May 2011, the ACIP measles, rubella, and mumps work group was formed to review and revise previously published vaccine recommendations. The work group held teleconference meetings monthly from May 2011 through October 2012. In addition to ACIP members, the work group included participants from the American Academy of Family Physicians (AAFP), the American Academy of Pediatrics (AAP), the American College Health Association, the Association of Immunization Managers, CDC, the Council of State and Territorial Epidemiologists, the Food and Drug Administration (FDA), the Infectious Diseases Society of America, the National Advisory Committee on Immunization (Canada), the National Institute of Health (NIH), and other infectious disease experts (7).*
Issues reviewed and considered by the work group included epidemiology of measles, rubella, CRS, and mumps in the United States; use of MMR vaccine among persons with HIV infection, specifically, revaccination of persons with perinatal HIV infection who were vaccinated before effective antiretroviral therapy (ART); use of a third dose of MMR vaccine for mumps outbreak control; timing of vaccine doses; use of immune globulin (IG) for measles postexposure prophylaxis; and vaccine safety. Recommendation options were developed and discussed by the work group. When evidence was lacking, the recommendations incorporated expert opinion of the work group members. Proposed revisions and a draft statement were presented to ACIP (ACIP meeting October 2011; February and June 2012) and approved at the October 2012 ACIP meeting. ACIP meeting minutes, including declaration of ACIP member conflicts of interest, if any, are available at http://www.cdc.gov/vaccines/acip/meetings/meetings-info.html.
Measles (rubeola) is classified as a member of the genus Morbillivirus in the family Paramyxoviridae. Measles is a highly contagious rash illness that is transmitted from person to person by direct contact with respiratory droplets or airborne spread. After exposure, up to 90% of susceptible persons develop measles. The average incubation period for measles is 10 to 12 days from exposure to prodrome and 14 days from exposure to rash (range: 7–21 days). Persons with measles are infectious 4 days before through 4 days after rash onset. In the United States, from 1987 to 2000, the most commonly reported complications associated with measles infection were pneumonia (6%), otitis media (7%), and diarrhea (8%) (8). For every 1,000 reported measles cases in the United States, approximately one case of encephalitis and two to three deaths resulted (9–11). The risk for death from measles or its complications is greater for infants, young children, and adults than for older children and adolescents. In low to middle income countries where malnutrition is common, measles is often more severe and the case-fatality ratio can be as high as 25% (12). In addition, measles can be severe and prolonged among immunocompromised persons, particularly those who have leukemias, lymphomas, or HIV infection (13–15). Among these persons, measles can occur without the typical rash and a patient can shed measles virus for several weeks after the acute illness (16–18). However, a fatal measles case without rash also has been reported in an apparently immunocompetent person (19).
Pregnant women also might be at high risk for severe measles and complications; however, available evidence does not support an association between measles in pregnancy and congenital defects (20). Measles illness in pregnancy might be associated with increased rates of spontaneous abortion, premature labor and preterm delivery, and low birthweight among affected infants (20–23).
A persistent measles virus infection can result in subacute sclerosing panencephalitis (SSPE), a rare and usually fatal neurologic degenerative disease. The risk for developing SSPE is 4–11 per 100,000 measles cases (24,25), but can be higher when measles occurs among children aged <2 years (25,26). Signs and symptoms of SSPE appear an average of 7 years after measles infection, but might appear decades later (27). Widespread use of measles vaccine has led to the virtual disappearance of SSPE in the United States, but imported cases still occur (28). Available epidemiologic and virologic data indicate that measles vaccine virus does not cause SSPE (27). Wild type measles virus nucleotide sequences have been detected consistently from persons with SSPE who have reported vaccination and no history of natural infection (24,29–34).
Before implementation of the national measles vaccination program in 1963, measles occurred in epidemic cycles and virtually every person acquired measles before adulthood (an estimated 3 to 4 million persons acquired measles each year). Approximately 500,000 persons with measles were reported each year in the United States, of whom 500 persons died, 48,000 were hospitalized, and another 1,000 had permanent brain damage from measles encephalitis (28).
After the introduction of the 1-dose measles vaccination program, the number of reported measles cases decreased during the late 1960s and early 1970s to approximately 22,000–75,000 cases per year (Figure 1) (35,36). Although measles incidence decreased substantially in all age groups, the greatest decrease occurred among children aged <10 years. During 1984 through 1988, an average of 3,750 cases was reported each year (37). However, measles outbreaks among school-aged children who had received 1 dose of measles vaccine prompted ACIP in 1989 to recommend that all children receive 2 doses of measles-containing vaccine, preferably as MMR vaccine (38,39). The second dose of measles-containing vaccine primarily was intended to induce immunity in the small percentage of persons who did not seroconvert after vaccination with the first dose of vaccine (primary vaccine failure).
During 1989 through 1991, a major resurgence of measles occurred in the United States. Approximately 55,000 cases and 120 measles-related deaths were reported. The resurgence was characterized by an increasing proportion of cases among unvaccinated preschool-aged children, particularly among those residing in urban areas (40,41). Efforts to increase vaccination coverage among preschool-aged children emphasized vaccination as close to the recommended age as possible. To improve access to ACIP-recommended vaccines, the Vaccines for Children program, a federally funded program that provides vaccines at no cost to eligible persons aged <19 years, was initiated in 1993 (42).
These efforts, combined with ongoing implementation of the 2-dose MMR vaccine recommendation, reduced reported measles cases to 309 in 1995 (43). During 1993, both epidemiologic and laboratory evidence suggested that transmission of indigenous measles had been interrupted in the United States (44,45).
The recommended measles vaccination schedule changed as knowledge of measles immunity increased and as the epidemiology of measles evolved within the United States. The recommended age for vaccination was 9 months in 1963, 12 months in 1965, and 15 months in 1967. In 1989, because of reported measles outbreaks among vaccinated school-aged children, ACIP and AAFP recommended 2 doses; with the first dose at age 15 months and the second dose at age 4 through 6 years, before school entry. In contrast, AAP had recommended administration of the second dose before middle school entry because outbreaks were occurring in older children, and to help reinforce the adolescent doctor's visit and counteract possible secondary vaccine failure (46). Since 1994, ages recommended by ACIP, AAFP, and AAP have been the same for the 2-dose MMR vaccine schedule; the first dose should be given to children aged 12 through 15 months and the second dose should be given to children aged 4 through 6 years (47).
Because of the success of the measles vaccination program in achieving and maintaining high 1-dose MMR vaccine coverage in preschool-aged children, high 2-dose MMR vaccine coverage in school-aged children, and improved measles control in the World Health Organization (WHO) Region of the Americas, measles was documented and verified as eliminated from the United States in 2000 (48). Elimination is defined as the absence of endemic transmission (i.e., interruption of continuous transmission lasting ≥12 months). In 2002, measles was declared eliminated from the WHO Region of the Americas (49).
Documenting and verifying the interruption of endemic transmission of the measles and rubella viruses in the Americas is ongoing in accordance with the Pan American Health Organization mandate of 2007 (http://www.paho.org/english/gov/csp/csp27.r2-e.pdf). An expert panel reviewed available data and unanimously agreed in December 2011 that measles elimination has been maintained in the United States (50,51). However, measles cases associated with importation of the virus from other countries continue to occur. From 2001 through 2011, a median of 63 measles cases (range: 37–220) and four outbreaks, defined as three or more cases linked in time or place (range: 2–17), were reported each year in the United States. Of the 911 cases, a total of 372 (41%) cases were importations, 804 (88%) were associated with importations, and 225 (25%) involved hospitalization. Two deaths were reported. Among the 162 cases reported from 2004 through 2008 among unvaccinated U.S. residents eligible for vaccination, a total of 110 (68%) were known to have occurred in persons who declined vaccination because of a philosophical, religious, or personal objection (52).
Rubella (German measles) is classified as a Rubivirus in the Togaviridae family. Rubella is an illness transmitted through direct or droplet contact from nasopharyngeal secretions and is characterized by rash, low-grade fever, lymphadenopathy, and malaise. Symptoms are often mild and up to 50% of rubella infections are subclinical (53,54). However, among adults infected with rubella, transient arthralgia or arthritis occurs frequently, particularly among women (55). Other complications occur infrequently; thrombocytopenic purpura occurs in approximately one out of 3,000 cases and is more likely to involve children (56), and encephalitis occurs in approximately one out of 6,000 cases and is more likely to involve adults (57,58).
Rubella infection in pregnant women, especially during the first trimester, can result in miscarriages, stillbirths, and CRS, a constellation of birth defects that often includes cataracts, hearing loss, mental retardation, and congenital heart defects. In addition, infants with CRS frequently exhibit both intrauterine and postnatal growth retardation. Infants who are moderately or severely affected by CRS are readily recognizable at birth, but mild CRS (e.g., slight cardiac involvement or deafness) might not be detected for months or years after birth or not at all. The risk for congenital infection and defects is highest during the first 12 weeks of gestation (59–62), and the risk for any defect decreases after the 12th week of gestation. Defects are rare when infection occurs after the 20th week (63). Subclinical maternal rubella infection also can cause congenital malformations. Fetal infection without clinical signs of CRS can occur during any stage of pregnancy.
Rubella reinfection can occur and has been reported after both wild type rubella infection and after receiving 1 dose of rubella vaccine. Asymptomatic maternal reinfection in pregnancy has been considered to present minimal risk to the fetus (congenital infection in <10%) (64), but several isolated reports have been made of fetal infection and CRS among infants born to mothers who had documented serologic evidence of rubella immunity before they became pregnant and had reinfection during the first 12 weeks of gestation (64–68). CRS was not reported when reinfection occurred after 12 weeks gestation (69–71).
Before licensure of live, attenuated rubella vaccines in the United States in 1969, rubella was common, and epidemics occurred every 6 to 9 years (72). Most rubella cases were among young children, with peak incidence among children aged 5 through 9 years (73). During the 1964 through 1965 rubella epidemic, an estimated 12.5 million rubella cases occurred in the United States, resulting in approximately 2,000 cases of encephalitis, 11,250 fetal deaths attributable to spontaneous or therapeutic abortions, 2,100 infants who were stillborn or died soon after birth, and 20,000 infants born with CRS (74).
After introduction of rubella vaccines in the United States in 1969, reported rubella cases declined 78%, from 57,686 in 1969 to 12,491 in 1976, and reported CRS cases declined by 69%, from 68 in 1970 to 23 in 1976 (Figure 2) (73). Rubella incidence declined in all age groups, but children aged <15 years experienced the greatest decline. Despite the declines, rubella outbreaks continued to occur among older adolescents and young adults and in settings where unvaccinated adults congregated. In 1977 and 1984, ACIP modified its recommendations to include vaccination of susceptible postpubertal females, adolescents, persons in military service, college students, and persons in certain work settings (75,76). The number of reported rubella cases decreased from 20,395 in 1977 to 225 in 1988, and CRS cases decreased from 29 in 1977 to 2 in 1988 (77).
During 1989 through 1991, a resurgence of rubella occurred, primarily because of outbreaks among unvaccinated adolescents and young adults who initially were not recommended for vaccination and in religious communities with low rubella vaccination coverage (77). As a result of the rubella outbreaks, two clusters of approximately 20 CRS cases occurred (78,79). Outbreaks during the mid-1990s occurred in settings where young adults congregated and involved unvaccinated persons who belonged to specific racial/ethnic groups (80). Further declines occurred as rubella vaccination efforts increased in other countries in the WHO Region of the Americas. From 2001 through 2004, reported rubella and CRS cases were at an all-time low, with an average of 14 reported rubella cases a year, four CRS cases, and one rubella outbreak (defined as three or more cases linked in time or place) (81).
In 2004, a panel convened by CDC reviewed available data and verified elimination of rubella in the United States (82). Rubella elimination is defined as the absence of endemic rubella transmission (i.e., continuous transmission lasting ≥12 months). From 2005 through 2011, a median of 11 rubella cases was reported each year in the United States (range: 4–18). In addition, two rubella outbreaks involving three cases, as well as four total CRS cases, were reported. Among the 67 rubella cases reported from 2005 through 2011, a total of 28 (42%) cases were known importations (83; CDC, unpublished data, 2012).
In 2010, on the basis of surveillance data, the Pan American Health Organization indicated that the WHO Region of the Americas had achieved the rubella and CRS elimination goals set in 2003 (84). Verification of maintenance of rubella elimination in the region is ongoing. However, an expert panel reviewed available data and unanimously agreed in December 2011 that rubella elimination has been maintained in the United States (50,51).
Mumps virus is a member of the genus Rubulavirus in the Paramyxoviridae family. Mumps is an acute viral infection characterized by fever and inflammation of the salivary glands. Parotitis is the most common manifestation, with onset an average of 16 to 18 days after exposure (range: 12–25 days). In some studies, mumps symptoms were described as nonspecific or primarily respiratory; however, these reports based findings on serologic results taken every 6 or 12 months, making it difficult to prove whether the respiratory tract symptoms were caused by mumps virus infection or if the symptoms happened to occur at the same time as the mumps infection (85,86). In other studies conducted during the prevaccine era, 15%–27% of infections were described as asymptomatic (85,87,88). In the vaccine era, it is difficult to estimate the number of asymptomatic infections because the way vaccine modifies clinical presentation is unclear and only clinical cases with parotitis, other salivary gland involvement, or mumps-related complications are notifiable. Serious complications can occur in the absence of parotitis (89,90). Results from an outbreak from 2009 through 2010 indicated that complications are lower in vaccinated patients than with unvaccinated patients (6); however, during an outbreak in 2006, vaccination status was not significantly associated with complications (91). Persons with mumps are most infectious around the time of parotitis onset (92). Complications of mumps infection can vary with age and sex.
In the prevaccine era, orchitis was reported in 12%–66% of postpubertal males infected with mumps (93,94), compared with U.S. outbreaks in 2006 and 2009 through 2010 in the vaccine era, during which the range of rates of orchitis among postpubertal males was 3%–10% (91,95,96). In 60%–83% of males with mumps orchitis, only one testis is affected (87,90). Sterility from mumps orchitis, even bilateral orchitis, occurs infrequently (93).
In the prevaccine era among postpubertal women, oophoritis was reported in approximately 5% of postpubertal females affected with mumps (97,98). Mastitis was included in case reports (99,100) but also was described in a 1956–1957 outbreak as affecting 31% of postpubertal females (87). A significant association between prepubescent mumps in females and infertility has been reported; it has been suggested that oophoritis might have resulted in a disturbance of follicular maturation (101). In the vaccine era, among postpubertal females, the range of oophoritis rates was ≤1% (91,95,96) and the range of mastitis rates was ≤1% (91,95,96).
In the prevaccine era, pancreatitis was reported in 4% of 342 persons infected with mumps in one community during a 2-year period (85) and was described in case reports (102,103). Mumps also was a major cause of hearing loss among children in the prevaccine era, which could be sudden in onset, bilateral, or permanent hearing loss (104–106). In the prevaccine era, clinical aseptic meningitis occurred in 0.02%–10% of mumps cases and typically was mild (85,88,107–109). However, in exceedingly rare cases, mumps meningoencephalitis can cause permanent sequelae, including severe ataxia (110). The incidence of mumps encephalitis ranged from one in 6,000 mumps cases (0.02%) (107) to one in 300 mumps cases (0.3%) in the prevaccine era (111). In the vaccine era, reported rates of pancreatitis, deafness, meningitis, and encephalitis were all <1% (91,95,96).
The average annual rate of hospitalization resulting from mumps during World War I was 55.8 per 1,000, which was exceeded only by the rates for influenza and gonorrhea (112). Mumps was a major cause of viral encephalitis, accounting for approximately 36% of encephalitis cases in 1967 (111). Death from mumps is exceedingly rare and is primarily caused by mumps-associated encephalitis (111). In the United States, from 1966 through 1971, two deaths occurred per 10,000 reported mumps cases (111). Among vaccinated persons, severe complications of mumps are uncommon but occur more frequently among adults than children. No mumps-related deaths were reported in the 2006 or the 2009–2010 U.S. outbreaks (91,95,96).
Among pregnant women with mumps during the first trimester, an increased rate of spontaneous abortion or intrauterine fetal death has been observed in some studies; however, no evidence indicates that mumps causes birth defects (87,113–116).
Before the introduction of vaccine in 1967, mumps was a universal disease of childhood. Most children were infected by age 14 years, with peak incidence among children aged 5 through 9 years (117,118). Outbreaks among the military were common, especially during times of mobilization (119,120).
Reported cases of mumps decreased steadily after the introduction of live mumps vaccine in 1967 and the recommendation in 1977 for routine vaccination (Figure 3) (121). However, from 1986 through 1987, a resurgence of mumps occurred when a cohort not targeted for vaccination and spared from natural infection by declining disease rates entered high school and college, resulting in 20,638 reported cases (122,123). By the early 2000s, on average, fewer than 270 cases were reported annually; a decrease of approximately 99% from the 152,209 cases reported in 1968, and seasonal peaks were no longer present (124). In 2006, an outbreak of 6,584 cases occurred and was centered among highly 2-dose vaccinated college students in the Midwestern United States (91). Children began receiving 2 doses of mumps vaccine after implementation of a 2-dose measles vaccination policy using MMR vaccine in 1989 (39). Nonetheless, ACIP specified in 2006 that all children and adults in certain high risk groups, including students at post-high school educational institutions, health-care personnel, and international travelers, should receive 2 doses of mumps-containing vaccine (3). From 2009 through 2010, mumps outbreaks occurred in a religious community in the Northeastern United States with approximately 3,500 cases and in the U.S. territory of Guam with 505 cases reported. Similar to the 2006 mumps outbreak, most patients had received 2 doses of MMR vaccine and were exposed in densely congregate settings (88,94). In 2011, a university campus in California reported 29 cases of mumps, of which 22 (76%) occurred among persons previously vaccinated with the recommended 2 doses of MMR vaccine (5).
Two combination vaccines are licensed and available in the United States to prevent measles, rubella, and mumps: trivalent MMR vaccine (measles-mumps-rubella [M-M-R II, Merck & Co., Inc.]) and quadrivalent MMRV vaccine (measles-mumps-rubella-varicella [ProQuad, Merck & Co., Inc.]). The efficacy and effectiveness of each component of the MMR vaccine is described below. MMRV vaccine was licensed on the basis of noninferior immunogenicity of the antigenic components compared with simultaneous administration of MMR vaccine and varicella vaccine (125). Formal studies to evaluate the clinical efficacy of MMRV vaccine have not been performed; efficacy of MMRV vaccine was inferred from that of MMR vaccine and varicella vaccine on the basis of noninferior immunogenicity (126). Monovalent measles, rubella, and mumps vaccines and other vaccine combinations are no longer commercially available in the United States.
The measles component of the combination vaccines that are currently distributed in the United States was licensed in 1968 and contains the live Enders-Edmonston (formerly called "Moraten") vaccine strain. Enders-Edmonston vaccine strain is a further attenuated preparation of a previous vaccine strain (Edmonston B) that is grown in chick embryo cell culture. Because of increased efficacy and fewer adverse reactions, the vaccine containing the Enders-Edmonston vaccine strain replaced previous vaccines: inactivated Edmonston vaccine (available in the United States from 1963 through 1976), live attenuated vaccines containing the Edmonston B (available in the United States from 1963 through 1975), and Schwarz strain (available in the United States from 1965 through 1976).
Measles-containing vaccines produce a subclinical or mild, noncommunicable infection inducing both humoral and cellular immunity. Antibodies develop among approximately 96% of children vaccinated at age 12 months with a single dose of the Enders-Edmonston vaccine strain (Table 1) (127–134). Almost all persons who do not respond to the measles component of the first dose of MMR vaccine at age ≥12 months respond to the second dose (135,136).
Data on early measles vaccination suggest that infants vaccinated at age 6 months might have an age-related delay in maturation of humoral immune response to measles vaccine, unrelated to passively transferred maternal antibody, compared with infants vaccinated at age 9 or 12 months (137,138). However, markers of cell-mediated immune response to measles vaccine were equivalent when infants were vaccinated at age 6, 9, and 12 months, regardless of presence of passive antibodies (139).
Although the cell-mediated immune response to the first dose of measles vaccine alone might not be protective, it might prime the humoral response to the second dose (140). Data indicate that revaccination of children first vaccinated as early as age 6 months will result in vaccine-induced immunity, although the response might be associated with a lower antibody titer than titers of children vaccinated at age 9 or 12 months (139).
One dose of measles-containing vaccine administered at age ≥12 months was approximately 94% effective in preventing measles (range: 39%–98%) in studies conducted in the WHO Region of the Americas (141,142). Measles outbreaks among populations that have received 2 doses of measles-containing vaccine are uncommon. The effectiveness of 2 doses of measles-containing vaccine was ≥99% in two studies conducted in the United States and 67%, 85%–≥94%, and 100% in three studies in Canada (142–146). The range in 2-dose vaccine effectiveness in the Canadian studies can be attributed to extremely small numbers (i.e., in the study with a 2-dose vaccine effectiveness of 67%, one 2-dose vaccinated person with measles and one unvaccinated person with measles were reported [145]). This range of effectiveness also can be attributed to age at vaccination (i.e., the 85% vaccine effectiveness represented children vaccinated at age 12 months, whereas the ≥94% vaccine effectiveness represented children vaccinated at age ≥15 months [146]). Furthermore, two studies found the incremental effectiveness of 2 doses was 89% and 94%, compared with 1 dose of measles-containing vaccine (145,147). Similar estimates of vaccine effectiveness have been reported from Australia and Europe (Table 1) (141).
Both serologic and epidemiologic evidence indicate that measles-containing vaccines induce long lasting immunity in most persons (148). Approximately 95% of vaccinated persons examined 11 years after initial vaccination and 15 years after the second dose of MMR (containing the Enders-Edmonston strain) vaccine had detectable antibodies to measles (149–152). In one study among 25 age-appropriately vaccinated children aged 4 through 6 years who had both low-level neutralizing antibodies and specific IgG antibodies by EIA before revaccination with MMR vaccine, 21 (84%) developed an anamnestic immune response upon revaccination; none developed IgM antibodies, indicating some level of immunity persisted (153).
The rubella component of the combination vaccines that are currently distributed in the United States was licensed in 1979 and contains the live Wistar RA 27/3 vaccine strain. The vaccine is prepared in human diploid cell culture and replaced previous vaccines (HPV-77 and Cendehill) because it induces a higher and more persistent antibody response and is associated with fewer adverse events (154–158).
Rubella vaccination induces both humoral and cellular immunity. Approximately 95% of susceptible persons aged ≥12 months developed serologic evidence of immunity to rubella after vaccination with a single dose of rubella vaccine containing the RA 27/3 strain (Table 1) (127,154,157–164). After a second dose of MMR vaccine, approximately 99% had detectable rubella antibody and approximately 60% had a fourfold increase in titer (165–167).
Outbreaks of rubella in populations vaccinated with the rubella RA 27/3 vaccine strains are rare. Available studies demonstrate that vaccines containing the rubella RA 27/3 strain are approximately 97% effective in preventing clinical disease after a single dose (range: 94%–100%) (Table 1) (168–170).
Follow-up studies indicate that 1 dose of rubella vaccine can provide long lasting immunity. The majority of persons had detectable rubella antibodies up to 16 years after 1 dose of rubella-containing vaccine, but antibody levels decreased over time (165,171–174). Although levels of vaccine-induced rubella antibodies might decrease over time, data from surveillance of rubella and CRS suggest that waning immunity with increased susceptibility to rubella disease does not occur. Among persons with 2 doses, approximately 91%–100% had detectable antibodies 12 to 15 years after receiving the second dose (150,165).
The mumps component of the vaccine available in the United States contains the live attenuated mumps Jeryl-Lynn vaccine strain. It was developed using an isolate from a child with mumps and passaged in embryonated hens' eggs and chick embryo cell cultures (175). The vaccine produces a subclinical, noncommunicable infection with very few side effects.
Approximately 94% of infants and children develop detectable mumps antibodies after vaccination with MMR vaccine (range: 89%–97%) (Table 1) (127,157,176–184). However, vaccination induces relatively low levels of antibodies compared with natural infection (185,186). Among persons who received a second dose of MMR vaccine, most mounted a secondary immune response, approximately 50% had a fourfold increase in antibody titers, and the proportion with low or undetectable titers was significantly reduced from 20% before vaccination with a second dose to 4% at 6 months post vaccination (187–189). Although antibody measurements are often used as a surrogate measure of immunity, no serologic tests are available for mumps that consistently and reliably predict immunity. The immune response to mumps vaccination probably involves both the humoral and cellular immune response, but no definitive correlates of protection have been identified.
Clinical studies conducted before vaccine licensure in approximately 7,000 children found a single dose of mumps vaccine to be approximately 95% effective in preventing mumps disease (186,190,191). However, vaccine effectiveness estimates have been lower in postlicensure studies. In the United States, mumps vaccine effectiveness has been estimated to be between 81% and 91% in junior high and high school settings (192–197), and between 64% and 76% among household or close contacts for 1 dose of mumps-containing vaccine (196,198). Population and school-based studies conducted in Europe and Canada report comparable estimates for vaccine effectiveness (49%–92%) (199–210).
Fewer studies have been conducted to assess the effectiveness of 2 doses of mumps-containing vaccine. In the United States, outbreaks among populations with high 2-dose coverage found 2 doses of mumps-containing vaccine to be 80%–92% effective in preventing clinical disease (198,211). In the 1988 through 1989 outbreak among junior high school students, the risk for mumps was five times higher for students who received 1 dose compared with students who received 2 doses (195). Population and school-based studies in Europe and Canada estimate 2 doses of mumps-containing vaccine to be 66%–95% effective (Table 1) (201–204,208–210). Despite relatively high 2-dose vaccine effectiveness, high 2-dose vaccine coverage might not be sufficient to prevent all outbreaks (6,91,212).
Studies indicate that 1 dose of MMR vaccine can provide persistent antibodies to mumps. The majority of persons (70%–99%) examined approximately 10 years after initial vaccination had detectable mumps antibodies (187–189). In addition, 70% of adults who were vaccinated in childhood had T-lymphocyte immunity to mumps compared with 80% of adults who acquired natural infection in childhood (213). Similarly, in 2-dose recipients, mumps antibodies were detectable in the majority of persons (74%–95%) followed over 12 years after receipt of a second dose of MMR vaccine, but antibody levels declined with time (150,187). Among vaccine recipients who do not have detectable mumps antibodies, mumps antigen-specific lymphoproliferative responses have been detected, but their role in protection against mumps disease is not clear (214,215).
For measles, evidence of the effectiveness of MMR or measles vaccine administered as postexposure prophylaxis is limited and mixed (216–222). Effectiveness might depend on timing of vaccination and the nature of the exposure. If administered within 72 hours of initial measles exposure, MMR vaccine might provide some protection against infection or modify the clinical course of disease (216–219,222).
Several published studies have compared attack rates among persons who received MMR or single antigen measles vaccine (without gamma globulin) as postexposure prophylaxis with those who remained unvaccinated after exposure to measles. Postexposure prophylaxis with MMR vaccine appears to be effective if the vaccine is administered within 3 days of exposure to measles in "limited" contact settings (e.g., schools, childcare, and medical offices) (218,222). Postexposure prophylaxis does not appear to be effective in settings with intense, prolonged, close contact, such as households and smaller childcare facilities, even when the dose is administered within 72 hours of rash onset, because persons in these settings are often exposed for long durations during the prodromal period when the index patient is infectious (219–221). However, these household studies are limited by number of persons receiving post-exposure prophylaxis (i.e., less than 10 persons were given MMR vaccine as postexposure prophylaxis within 72 hours of rash onset in each of the cited studies) (219–221). Revaccination within 72 hours of exposure of those who have received 1 dose before exposure also might prevent disease (223). For rubella and mumps, postexposure MMR vaccination has not been shown to prevent or alter the clinical severity of disease.
Data on use and effectiveness of a third dose of MMR vaccine for mumps outbreak control are limited. A study among a small number of seronegative college students who had 2 documented doses of MMR vaccine demonstrated that a third dose of MMR vaccine resulted in a rapid mumps virus IgG response. Of 17 participants, a total of 14 (82%) were IgG positive at 7–10 days after revaccination, suggesting that previously vaccinated persons administered a third dose of MMR vaccine had the capacity to mount a rapid anamnestic immune response that could possibly boost immunity to protective levels (224). In 2010, in collaboration with local health departments, CDC conducted two Institutional Review Board (IRB)-approved studies to evaluate the effect of a third dose of MMR vaccine during mumps outbreaks in highly vaccinated populations in Orange County, New York (>94% 2-dose coverage among 2,688 students attending private school in grades 6 through12) and Guam (≥95% 2-dose coverage among 3,364 students attending public primary and middle school in grades 4 through 8).
In Orange County, New York, a total of 1,755 (81%) eligible students in grades 6 through 12 (ages 11 through 17 years) in three schools received a third dose of MMR vaccine as part of the study (95). Overall attack rates declined 76% in the village after the intervention, with the greatest decline among those aged 11 through 17 years targeted for vaccination (with a significant decline of 96% postintervention compared with preintervention). The 96% decline in attack rates in this age group was significantly greater than the declines in other age groups that did not receive the third dose intervention (95). However, the intervention was conducted after the outbreak started to decline. Because of the high rate of vaccine uptake and small number of cases observed in the 22–42 days after vaccination, the study could not directly evaluate the effectiveness of a third dose.
During a mumps outbreak in Guam in 2010, a total of 3,239 eligible children aged 9 through 14 years in seven schools were offered a third dose of MMR vaccine (96). Of the eligible children, 1,067 (33%) received a third dose of MMR vaccine. More than one incubation period after the third dose intervention, students who had 3 doses of MMR vaccine had a 2.6-fold lower mumps attack rate compared with students who had 2 doses of MMR vaccine (0.9 per 1,000 versus 2.4 per 1,000), but the difference was not statistically significant (Relative Risk [RR] = 0.40, 95% Confidence interval [CI] = 0.05–3.4, p = 0.67). The intervention was conducted after the outbreak started to decline and during the week before the end of the school year, which limited the ability to evaluate effectiveness of the intervention.
Data are insufficient to recommend for or against the use of a third dose of MMR vaccine for mumps outbreak control. CDC has issued guidance for consideration for use of a third dose in specifically identified target populations along with criteria for public health departments to consider for decision making (http://www.cdc.gov/vaccines/pubs/surv-manual/chpt09-mumps.html).
Before the availability of effective ART, responses to MMR vaccine among persons with HIV infection were suboptimal. Although response to revaccination varied, it generally was poor (225,226). In addition, measles antibodies appear to decline more rapidly in children with HIV infection than in children without HIV infection (227,228).
Memory B cell counts and function appear to be normal in HIV-infected children who are started on effective ART early (aged <1 year), and responses to measles and rubella vaccination appear to be adequate. Measles antibody titers were higher in HIV-infected children who started effective ART early compared with HIV-infected children who started effective ART later in life (229). Likewise, vaccinated HIV-infected children who initiated effective ART before vaccination had rubella antibody responses similar to those observed in HIV-uninfected children (230).
Despite evidence of immune reconstitution, effective ART does not appear to reliably restore immunity from previous vaccinations. Perinatally HIV-infected youth who received MMR vaccine before effective ART might have increased susceptibility to measles, mumps, and rubella compared with HIV-exposed but uninfected persons. Approximately 45%–65% of previously vaccinated HIV-infected children had detectable antibodies to measles after initiation of effective ART, 55%–80% had detectable antibodies to rubella, and 52%–59% had detectable antibodies to mumps (231–235). However, revaccination with MMR vaccine after initiation of effective ART increased the proportion of HIV-infected children with detectable antibodies to measles, rubella, and mumps (64%–90% for measles, 80%–100% for rubella, and 78% for mumps) (230,234,236–240). Although, data on duration of response to revaccination on effective ART are limited, the majority of children had detectable antibodies to measles (73%–85%), rubella (79%), and mumps (61%) 1–4 years after revaccination (234,238,240).
The lyophilized live MMR vaccine and MMRV vaccine should be reconstituted and administered as recommended by the manufacturer (241,242). Both vaccines available in the United States should be administered subcutaneously. Although both vaccines must be protected from light, which might inactivate the vaccine viruses, the two vaccines have different storage requirements (Table 2). Administration of improperly stored vaccine might fail to provide protection against disease. The diluent can be stored in the refrigerator or at room temperature but should not be allowed to freeze.
MMR vaccine is supplied in lyophilized form and must be stored at −50°C to 8°C (−58°F to 46°F) and protected from light at all times. The vaccine in the lyophilized form can be stored in the freezer. Reconstituted MMR vaccine should be used immediately or stored in a dark place at 2°C to 8°C (36°F to 46°F) for up to 8 hours and should not be frozen or exposed to freezing temperatures (241).
MMRV vaccine is supplied in a lyophilized frozen form that should be stored at −50°C to -15°C (−58°F to 5°F) in a reliable freezer. Reconstituted vaccine can be stored at room temperature between 20°C to 25°C (68°F to 77°F), protected from light for up to 30 minutes. Reconstituted MMRV vaccine must be discarded if not used within 30 minutes and should not be frozen (242).
Before administering MMR or MMRV vaccine, providers should consult the package insert for precautions, warnings, and contraindications (241,242).
Contraindications for MMR and MMRV vaccines include history of anaphylactic reactions to neomycin, history of severe allergic reaction to any component of the vaccine, pregnancy, and immunosuppression.
History of anaphylactic reactions to neomycin. MMR and MMRV vaccine contain trace amounts of neomycin; therefore, persons who have experienced anaphylactic reactions to topically or systemically administered neomycin should not receive these vaccines. However, neomycin allergy usually manifests as a delayed type or cell-mediated immune response (i.e., a contact dermatitis) rather than as anaphylaxis. In persons who have such sensitivity, the adverse reaction to the neomycin in the vaccine is an erythematous, pruritic nodule or papule appearing 48–72 hours after vaccination (243). A history of contact dermatitis to neomycin is not a contraindication to receiving MMR-containing vaccine.
History of severe allergic reaction to any component of the vaccine. MMR and MMRV vaccine should not be administered to persons who have experienced severe allergic reactions to a previous dose of measles-, mumps-, rubella-, or varicella (for MMRV vaccine)-containing vaccine or to a vaccine component. Although measles and mumps components of the vaccine are grown in chick embryo fibroblast tissue culture, allergy to egg is not a contraindication to vaccination. Among persons who are allergic to eggs, the risk for serious allergic reactions, such as anaphylaxis after administration of MMR vaccine, is exceedingly low (i.e., at least 99% of children with challenge-proved egg allergy can receive this vaccine in one subcutaneous dose without severe anaphylactic reactions [CI = 99%–100%]) (244). Skin testing with vaccine is not predictive of allergic reaction to vaccination (244–246). Therefore, skin testing is not required before administering MMR or MMRV vaccines to persons who are allergic to eggs. The rare serious allergic reactions after measles or mumps vaccination or MMR vaccination are not believed to be caused by egg antigens, but by other components of the vaccine (247–249)
Pregnancy. MMR vaccines should not be administered to women known to be pregnant or attempting to become pregnant. Because of the theoretical risk to the fetus when the mother receives a live virus vaccine, women should be counseled to avoid becoming pregnant for 28 days after receipt of MMR vaccine (2). If the vaccine is inadvertently administered to a pregnant woman or a pregnancy occurs within 28 days of vaccination, she should be counseled about the theoretical risk to the fetus. The theoretical maximum risk for CRS after the administration of rubella RA 27/3 vaccine on the basis of the 95% CI of the binomial distribution with 144 observations in one study was estimated to be 2.6%, and the observed risk was 0% (250). Other reports have documented no cases of CRS among approximately 1,000 live-born infants of susceptible women who were vaccinated inadvertently with the rubella RA 27/3 vaccine while pregnant or just before conception (251–257). Of these, approximately 100 women were known to be vaccinated within 1 week before to 4 weeks after conception (251,252), the period presumed to be the highest risk for viremia and fetal malformations. These figures are considerably lower than the ≥20% risk associated with wild rubella virus infection of mothers during the first trimester of pregnancy with wild rubella virus or the risk for non-CRS-induced congenital defects in pregnancy (250). Thus, MMR vaccination during pregnancy should not be considered an indication for termination of pregnancy.
MMR vaccine can be administered safely to children or other persons without evidence of immunity to measles, mumps, or rubella and who have pregnant household contacts to help protect these pregnant women from exposure to wild rubella virus. No reports of transmission of measles or mumps vaccine virus exist from vaccine recipients to susceptible contacts; although small amounts of rubella vaccine virus are detected in the noses or throats of most rubella susceptible persons 7 to 28 days post-vaccination, no documented confirmed cases of transmission of rubella vaccine virus have been reported.
Immunosuppression. MMR and MMRV vaccine should not be administered to 1) persons with primary or acquired immunodeficiency, including persons with immunosuppression associated with cellular immunodeficiencies, hypogammaglobulinemia, dysgammaglobulinemia and AIDS or severe immunosuppression associated with HIV infection; 2) persons with blood dyscrasias, leukemia, lymphomas of any type, or other malignant neoplasms affecting the bone marrow or lymphatic system; 3) persons who have a family history of congenital or hereditary immunodeficiency in first-degree relatives (e.g., parents and siblings), unless the immune competence of the potential vaccine recipient has been substantiated clinically or verified by a laboratory; or 4) persons receiving systemic immunosuppressive therapy, including corticosteroids ≥2 mg/kg of body weight or ≥20 mg/day of prednisone or equivalent for persons who weigh >10 kg, when administered for ≥2 weeks (258). Persons with HIV infection who do not have severe immunosuppression should receive MMR vaccine, but not MMRV vaccine (see subsection titled Persons with HIV Infection). Measles inclusion body encephalitis has been reported after administration of MMR vaccine to immunosuppressed persons, as well as after natural measles infection with wild type virus (see section titled Safety of MMR and MMRV Vaccines) (259–261).
Precautions for MMR and MMRV vaccines include recent (≤11 months) receipt of an antibody-containing blood product, concurrent moderate or severe illness with or without fever, history of thrombocytopenia or thrombocytopenic purpura, and tuberculin skin testing. If a tuberculin test is to be performed, it should be administered either any time before, simultaneously with, or at least 4–6 weeks after administration of MMR or MMRV vaccine. An additional precaution for MMRV vaccine includes persons with a personal or family history of seizures of any etiology.
Recent (≤11 months) receipt of antibody-containing blood product. Receipt of antibody-containing blood products (e.g., IG, whole blood, or packed red blood cells) might interfere with the serologic response to measles and rubella vaccine for variable periods, depending on the dose of IG administered (262). The effect of IG-containing preparations on the response to mumps vaccine is unknown.
MMR vaccine should be administered to persons who have received an IG preparation only after the recommended intervals have elapsed (258). However, postpartum administration of MMR vaccine to women who lack presumptive evidence of immunity to rubella should not be delayed because anti-Rho(D) IG (human) or any other blood product were received during the last trimester of pregnancy or at delivery. These women should be vaccinated immediately after delivery and tested at least 3 months later to ensure that they have presumptive evidence of immunity to rubella and measles.
Moderate or severe illness with or without fever. Vaccination of persons with concurrent moderate or severe illness, including untreated, active tuberculosis, should be deferred until they have recovered. This precaution avoids superimposing any adverse effects of the vaccine on the underlying illness or mistakenly attributing a manifestation of the underlying illness to the vaccine. The decision to vaccinate or postpone vaccination depends largely on the cause of the illness and the severity of symptoms. MMR vaccine can be administered to children who have mild illness, with or without low-grade fever, including mild upper respiratory infections, diarrhea, and otitis media. Data indicate that seroconversion is not affected by concurrent or recent mild illness (263–265). Physicians should be alert to the vaccine-associated temperature elevations that might occur predominately in the second week after vaccination, especially with the first dose of MMRV vaccine.
Persons being treated for tuberculosis have not experienced exacerbations of the disease when vaccinated with MMR vaccine. Although no studies have been reported concerning the effect of MMR or MMRV vaccines on persons with untreated tuberculosis, a theoretical basis exists for concern that measles vaccine might exacerbate tuberculosis. Consequently, before administering MMR vaccine to persons with untreated active tuberculosis, initiating antituberculous therapy is advisable. Testing for latent tuberculosis infection is not a prerequisite for routine vaccination with MMR vaccine.
History of thrombocytopenia or thrombocytopenic purpura. Persons who have a history of thrombocytopenia or thrombocytopenic purpura might be at increased risk for developing clinically significant thrombocytopenia after MMR or MMRV vaccination. Persons with a history of thrombocytopenia have experienced recurrences after MMR vaccination (266,267), whereas others have not had a repeat episode after MMR vaccination (268–270). In addition, persons who developed thrombocytopenia with a previous dose might develop thrombocytopenia with a subsequent dose of MMR vaccine (271,272). However, among 33 children who were admitted for idiopathic thrombocytopenic purpura before receipt of a second dose of MMR vaccine, none had a recurrence within 6 weeks of the second MMR vaccine (273). Serologic evidence of immunity can be sought to determine whether or not an additional dose of MMR or MMRV vaccine is needed.
Tuberculin testing. MMR vaccine might interfere with the response to a tuberculin skin test, resulting in a temporary depression of tuberculin skin sensitivity (274–276). Therefore, if a tuberculin skin test is to be performed, it should be administered either any time before, simultaneously with, or at least 4–6 weeks after MMR or MMRV vaccine. As with the tuberculin skin tests, live virus vaccines also might affect tuberculosis interferon-gamma release assay (IGRAs) test results. However, the effect of live virus vaccination on IGRAs has not been studied. Until additional information is available, IGRA testing in the context of live virus vaccine administration should be done either on the same day as vaccination with live-virus vaccine or 4–6 weeks after the administration of the live-virus vaccine.
Personal or family history of seizures of any etiology. A personal or family (i.e., sibling or parent) history of seizures of any etiology is a precaution for the first dose of MMRV but not MMR vaccination. Studies suggest that children who have a personal or family history of febrile seizures or family history of epilepsy are at increased risk for febrile seizures compared with children without such histories. In one study, the risk difference of febrile seizure within 14 days of MMR vaccination for children aged 15 to 17 months with a personal history of febrile seizures was 19.5 per 1,000 (CI = 16.1– 23.6) and for siblings of children with a history of febrile seizures was four per 1,000 (CI = 2.9–5.4) compared with unvaccinated children of the same age (277). In another study, the match adjusted odds ratio for children with a family history of febrile seizures was 4.8 (CI = 1.3–18.6) compared with children without a family history of febrile seizures (278). For the first dose of measles vaccine, children with a personal or family history of seizures of any etiology generally should be vaccinated with MMR vaccine because the risks for using MMRV vaccine in this group of children generally outweigh the benefits.
MMR vaccine generally is well-tolerated and rarely associated with serious adverse events. MMR vaccine might cause fever (<15%), transient rashes (5%), transient lymphadenopathy (5% of children and 20% of adults), or parotitis (<1%) (160,163,279–283). Febrile reactions usually occur 7–12 days after vaccination and generally last 1–2 days (280). The majority of persons with fever are otherwise asymptomatic. Four adverse events (i.e., coryza, cough, pharyngitis, and headache) after revaccination were found to be significantly lower with a second dose of MMR vaccine, and six adverse events (i.e., conjunctivitis, nausea, vomiting, lymphadenopathy, joint pain, and swollen jaw) had no significant change compared with the prevaccination baseline in school-aged children (284).
Expert committees at the Institute of Medicine (IOM) reviewed evidence concerning the causal relation between MMR vaccination and various adverse events (285–289). Their causality was assessed on the basis of epidemiologic evidence derived from studies of populations, as well as mechanistic evidence derived primarily from biologic and clinical studies in animals and humans; risk was not quantified. IOM determined that evidence supports a causal relation between MMR vaccination and anaphylaxis, febrile seizures, thrombocytopenic purpura, transient arthralgia, and measles inclusion body encephalitis in persons with demonstrated immunodeficiencies.
Anaphylaxis. Immediate anaphylactic reactions after MMR vaccination are rare (1.8–14.4 per million doses) (290–293). Although measles- and mumps-containing vaccines are grown in tissue from chick embryos, the rare serious allergic reactions after MMR vaccination are not believed to be caused by egg antigens but by other components of the vaccine, such as gelatin or neomycin (247–249).
Febrile seizures. MMR vaccination might cause febrile seizures. The risk for such seizures is approximately one case for every 3,000 to 4,000 doses of MMR vaccine administered (294,295). Children with a personal or family history of febrile seizures or family history of epilepsy might be at increased risk for febrile seizures after MMR vaccination (277,278). The febrile seizures typically occur 6–14 days after vaccination and do not appear to be associated with any long-term sequelae (294–297). An approximate twofold increased risk exists for febrile seizures among children aged 12 to 23 months who received the first dose of MMRV vaccine compared with children who received MMR and varicella vaccines separately. One additional febrile seizure occurred 5 through 12 days after vaccination per 2,300 to 2,600 children who received the first dose of MMRV vaccine compared with children who received the first dose of MMR and varicella vaccine separately but at the same visit (298,299). No increased risk for febrile seizures was observed after vaccination with MMRV vaccine in children aged 4 through 6 years (300). For additional details, see ACIP recommendations on the use of combination MMRV vaccine (126).
Thrombocytopenic purpura. Immune thrombocytopenic purpura (ITP), a disorder affecting blood platelet count, might be idiopathic or associated with a number of viral infections. ITP after receipt of live attenuated measles vaccine and wild type measles infections is usually self-limited and not life threatening; however, complications of ITP might include severe bleeding requiring blood transfusion (267,268,270). The risk for ITP increases during the 6 weeks after MMR vaccination, with one study estimating one case per 40,000 doses (270). The risk for thrombocytopenia after MMR vaccination is much less than after natural infection with rubella (one case per 3,000 infections) (56). On the basis of case reports, the risk for MMR vaccine-associated thrombocytopenia might be increased for persons who previously have had ITP (see Precautions).
Arthralgia and arthritis. Joint symptoms are associated with the rubella component of MMR vaccine (301). Among persons without rubella immunity who receive rubella-containing vaccine, arthralgia and transient arthritis occur more frequently among adults than children, and more frequently among postpubertal females than males (302,303). Acute arthralgia or arthritis are rare among children who receive RA 27/3 vaccine (160,303). In contrast, arthralgia develops among approximately 25% of nonimmune postpubertal females after vaccination with rubella RA 27/3 vaccine, and approximately 10% to 30% have acute arthritis-like signs and symptoms (154,160,282,301). Arthralgia or arthritis generally begin 1–3 weeks after vaccination, usually are mild and not incapacitating, lasts about 2 days, and rarely recur (160,301,303,304).
Measles inclusion body encephalitis. Measles inclusion body encephalitis is a complication of measles infection that occurs in young persons with defective cellular immunity from either congenital or acquired causes. The complications develop within 1 year after initial measles infection and the mortality rate is high. Three published reports in persons with immune deficiencies described measles inclusion body encephalitis after measles vaccination, documented by intranuclear inclusions corresponding to measles virus or the isolation of measles virus from the brain among vaccinated persons (259–261,289). The time from vaccination to development of measles inclusion body encephalitis for these cases was 4–9 months, consistent with development of measles inclusion body encephalitis after infection with wild measles virus (305). In one case, the measles vaccine strain was identified (260).
Other possible adverse events. IOM concluded that the body of evidence favors rejection of a causal association between MMR vaccine and risk for autistic spectrum disorders (ASD), including autism, inflammatory bowel diseases, and type 1 diabetes mellitus. In addition, the available evidence was not adequate to accept or reject a causal relation between MMR vaccine and the following conditions: acute disseminated encephalomyelitis, afebrile seizures, brachial neuritis, chronic arthralgia, chronic arthritis, chronic fatigue syndrome, chronic inflammatory disseminated polyneuropathy, encephalopathy, fibromyalgia, Guillain-Barré syndrome, hearing loss, hepatitis, meningitis, multiple sclerosis, neuromyelitis optica, optic neuritis, transverse myelitis, opsoclonus myoclonus syndrome, or radiculoneuritis and other neuropathies.
Short-term safety of administration of a third dose of MMR vaccine was evaluated following vaccination clinics during two mumps outbreaks among 2,130 persons aged 9 through 21 years (96,306). Although these studies did not include a control group, few adverse events were reported after administration of a third dose of MMR vaccine (7% in Orange County, New York and 6% in Guam). The most commonly reported adverse events were pain, redness, or swelling at the injection site (2%–4%); joint or muscle aches (2%–3%); and dizziness or lightheadedness (2%). No serious adverse events were reported in either study.
HIV-infected persons are at increased risk for severe complications if infected with measles (16,307–310), and several severe and fatal measles cases have been reported in HIV-infected children after vaccination, including progressive measles pneumonitis in a person with HIV infection and severe immunosuppression who received MMR vaccine (311), and several deaths after measles vaccination among persons with severe immunosuppression unrelated to HIV infection (312–314). No serious or unusual adverse events have been reported after measles vaccination among persons with HIV infection who did not have evidence of severe immunosuppression (315–320). Severe immunosuppression is defined as CD4+ T-lymphocyte percentages <15% at any age or CD4 count <200 lymphocytes/mm3 for persons aged >5 years (321,322). Furthermore, no serious adverse events have been reported in several studies in which MMR vaccine was administered to a small number of children on ART with histories of immunosuppression (231,233,238). MMR vaccine is not recommended for persons with HIV infection who have evidence of severe immunosuppression, and MMRV vaccine is not approved for use in any persons with HIV infection.
Clinically significant adverse events that arise after vaccination should be reported to the Vaccine Adverse Event Reporting System (VAERS) at http://vaers.hhs.gov/esub/index. VAERS is a postmarketing safety surveillance program that collects information about adverse events (possible side effects) that occur after the administration of vaccines licensed for use in the United States.
Reports can be filed securely online, by mail, or by fax. A VAERS form can be downloaded from the VAERS website or requested by e-mail (info@vaers.org), telephone (800-822-7967), or fax (877-721-0366). Additional information on VAERS or vaccine safety is available at http://vaers.hhs.gov/about/index or by calling telephone 800-822-7967.
The National Vaccine Injury Compensation Program (VICP), established by the National Childhood Vaccine Injury Act (NCVIA) of 1986, as amended, provides a mechanism through which compensation can be paid on behalf of a person determined to have been injured or to have died as a result of receiving a vaccine covered by VICP (323). NCVIA requires health-care providers to report any adverse events listed by the manufacturer as a contraindication to further vaccine or any adverse event listed in the VAERS Table of Reportable Events Following Vaccination that occurs within the specified time period after vaccination (324). The Vaccine Injury Table lists the vaccines covered by VICP and the injuries and conditions (including death) for which compensation might be paid. If the injury or condition is not included in the table, or does not occur within the specified time period on the table, persons must prove that the vaccine caused the injury or condition. For a person to be eligible for compensation, the general filing deadlines for injuries require claims to be filed within 3 years after the first symptom of the vaccine injury; for a death, claims must be filed within 2 years of the vaccine-related death and not more than 4 years after the start of the first symptom of the vaccine-related injury from which the death occurred. When a new vaccine is covered by VICP or when a new injury/condition is added to the table, claims that do not meet the general filing deadlines must be filed within 2 years from the date the vaccine or injury/condition is added to the table for injuries or deaths that occurred up to 8 years before the table change. Persons who receive a VICP-covered vaccine might be eligible to file a claim. Additional information about VICP is available at http://www.hrsa.gov/vaccinecompensation/index.html or by calling 800–338–2382.
Human immune globulin (IG) is a blood product used to provide antibodies for short-term prevention of infectious diseases, including measles. IG products are prepared from plasma pools derived from thousands of donors. Persons who have measles disease typically have higher measles antibody titers than persons who have vaccine-induced measles immunity. Although the prevalence of measles antibodies is high in the U.S. population (325), potency of IG products has declined as a result of change in the donor population from persons with immunity from disease to persons with predominately vaccine-induced measles immunity (326).
Multiple IG preparations are available in the United States and include IG administered intramuscularly (IGIM), intravenously (IGIV), and subcutaneously (IGSC). The minimum measles antibody potency requirement for IGIM used in the United States is 0.60 of the reference standard (U.S. Reference IG, Lot 176) and 0.48 of the reference standard for IGIV and IGSC. In 2007, the FDA Blood Products Advisory Committee lowered the measles antibody concentration requirements for IGIV and IGSC from 0.60 to 0.48 of the reference standard when testing and calculations indicated that IGIV and IGSC products with this minimum potency could be expected to provide a measles antibody concentration of ≥120 mIU/mL, the estimated protective level of measles neutralizing antibody (327), for 28–30 days, if administered at the minimum label recommended dose of 200 mg/kg (328).
Historically, IGIM has been the blood product of choice for short-term measles prophylaxis and was the product used to demonstrate efficacy for measles postexposure prophylaxis (329). The recommended dose of IGIM is 0.5mL/kg. Because concentrations of antibodies are lower, an increase in dose is needed. However, postexposure use of IGIM might be limited because of volume limitations. The maximum dose by volume is 15 mL. Persons who weigh >30 kg will receive less than the recommended dose and will have lower titers than recommended.
IGIV has been available since 1981 and is used primarily for the prevention of common infectious diseases for patients with primary immunodeficiency disorders. Although a larger dose can be administered with IGIV compared with IGIM, clinical use of IGIV has important disadvantages, including high cost and administration requiring extended observation in specialized settings by skilled professionals (i.e., hospital setting).
IGSC has been available since 2006 with the same major indication as IGIV. However, administration requires a pump and advanced training. Also, multiple, consecutive weekly doses are needed to establish a steady-state with protective antibody levels.
Additional information on licensed IG products is available at http://www.fda.gov/BiologicsBloodVaccines/BloodBloodProducts/ApprovedProducts/LicensedProductsBLAs/FractionatedPlasmaProducts/ucm127589.htm. One IGIM product is licensed and available in the United States, and the package insert is available at http://www.talecris-pi.info/inserts/gamastans-d.pdf.
IGIM has been used as prophylaxis to prevent or attenuate measles disease since the 1940s, when it was demonstrated that IGIM can reduce the risk for measles or modify disease if administered within 6 days of exposure (329,330) with a dose response effect (331). However, postexposure IGIM was not effective in a study conducted in 1990 (220). Although the optimal dose of IGIM needed to provide protection against measles infection after exposure is unknown, a study from 1999 through 2000 indicated a titer-dependent effect, with higher antimeasles titer providing the greatest protection (332). Children who did not develop disease received a mean dose of 10.9 IU/kg compared with 5.7 IU/kg for children in which postexposure prophylaxis with IGIM failed.
Infants typically are protected from measles at birth by passively acquired maternal antibodies. The duration of this protection depends largely on the amount of antibody transferred, which is related to gestational age and maternal antibody titer (333). Women with vaccine-derived measles immunity have lower antibody titers and transfer shorter term protection than women who have had measles disease (333–335). Although foreign-born mothers accounted for 23% of all births in 2010 and most of these mothers born outside the Western Hemisphere likely had immunity from wild measles (336), the majority of women of childbearing age in the United States now have vaccine-derived measles immunity. Fewer opportunities exist for boosting this immunity by exposure to wild type viruses. Thus, infants born now are more likely to be susceptible to measles at a younger age (337). Seroepidemiologic studies indicate that 7% of infants born in the United States might lack antimeasles antibodies at birth and up to 90% of infants might be seronegative by age 6 months (139,325). These data suggest a change in the window of vulnerability for measles infection during infancy, a strong need to preserve herd protection, vigilance for imported cases, and rapid access to IG products when postexposure prophylaxis is needed.
The criteria for acceptable evidence of measles, rubella, and mumps immunity were developed to guide vaccination assessment and administration in clinical and public health settings and to provide presumptive rather than absolute evidence of immunity. Persons who meet the criteria for acceptable evidence of immunity have a very high likelihood of immunity. Occasionally, a person who meets the criteria for presumptive immunity can acquire and transmit disease. Specific criteria for documentation of immunity have been established for measles, rubella, and mumps (Table 3). These criteria apply only to routine vaccination. During outbreaks, recommended criteria for presumptive evidence of immunity might differ for some groups (see section titled Recommendations during Outbreaks of Measles, Rubella, or Mumps).
Vaccine doses with written documentation of the date of administration at age ≥12 months are the only doses considered to be valid. Self-reported doses and history of vaccination provided by a parent or other caregiver are not considered adequate evidence of immunity. Because of the extremely low incidence of these diseases in the United States, the validity of clinical diagnosis of measles, rubella, and mumps is questionable and should not be considered in assessing evidence. Persons who do not have documentation of adequate vaccination or other acceptable evidence of immunity (Table 3) should be vaccinated.
Serologic screening for measles, rubella, or mumps immunity before vaccination is not necessary and not recommended if a person has other acceptable evidence of immunity to these diseases (Table 3). Similarly, postvaccination serologic testing to verify an immune response is not recommended.
Documented age-appropriate vaccination supersedes the results of subsequent serologic testing. If a person who has 2 documented doses of measles- or mumps-containing vaccines is tested serologically and is determined to have negative or equivocal measles or mumps titer results, it is not recommended that the person receive an additional dose of MMR vaccine. Such persons should be considered to have presumptive evidence of immunity. In the event that a person who has 1 dose of rubella-containing vaccine is tested serologically and is determined to have negative or equivocal rubella titer results, it is not recommended that the person receive an additional dose of MMR vaccine, except for women of childbearing age. Women of childbearing age who have 1 or 2 documented doses of rubella-containing vaccine and have rubella-specific IgG levels that are not clearly positive should be administered 1 additional dose of MMR vaccine (maximum of 3 doses) and do not need to be retested for serologic evidence of rubella immunity.
Persons who have documentation of adequate vaccination for measles at age ≥12 months, laboratory evidence of measles immunity, laboratory confirmation of disease, or were born before 1957 have acceptable presumptive evidence of measles immunity (Table 3). Adequate vaccination for measles for preschool-aged children (i.e., aged ≥12 months) and adults not at high risk for exposure or transmission is documentation of vaccination with at least 1 dose of live measles virus-containing vaccine. For school-aged children in kindergarten through grade 12, students at post-high school educational institutions, health-care personnel, and international travelers, adequate vaccination for measles is documentation of vaccination with 2 doses of live measles virus-containing vaccine separated by at least 28 days. Adequate vaccination for measles for infants aged 6 through 11 months before international travel is 1 dose of live measles virus-containing vaccine.
Persons who have measles-specific IgG antibody that is detectable by any commonly used serologic assay are considered to have adequate laboratory evidence of measles immunity. Persons with an equivocal serologic test result do not have adequate presumptive evidence of immunity and should be considered susceptible, unless they have other evidence of measles immunity (Table 3) or subsequent testing indicates measles immunity.
Persons who have documentation of vaccination with at least 1 dose of live rubella virus-containing vaccine at age ≥12 months, laboratory evidence of rubella immunity, laboratory confirmation of disease, or were born before 1957 (except women who could become pregnant) have acceptable presumptive evidence of rubella immunity (Table 3). Birth before 1957 is not acceptable evidence of rubella immunity for women who could become pregnant. Documented evidence of rubella immunity is important for women who could become pregnant because rubella can occur among some unvaccinated persons born before 1957 and congenital rubella and CRS can occur among the offspring of women infected with rubella during pregnancy.
Persons who have rubella-specific antibody levels above the standard positive cutoff value for the assay can be considered to have adequate evidence of rubella immunity. Except for women of childbearing age, persons who have an equivocal serologic test result should be considered susceptible to rubella unless they have documented receipt of 1 dose of rubella-containing vaccine or subsequent serologic test results indicate rubella immunity. Vaccinated women of childbearing age who have received 1 or 2 doses of rubella-containing vaccine and have rubella serum IgG levels that are not clearly positive should be administered 1 additional dose of MMR vaccine (maximum of 3 doses) and do not need to be retested for serologic evidence of rubella immunity.
Persons who have written documentation of adequate vaccination for mumps at age ≥12 months, laboratory evidence of mumps immunity, laboratory confirmation of disease, or were born before 1957 have acceptable presumptive evidence of mumps immunity (Table 3). Adequate vaccination for mumps for preschool-aged children (i.e., aged ≥12 months) and adults not at high risk for exposure or transmission is documentation of vaccination with at least 1 dose of live mumps virus-containing vaccine. For children in kindergarten through grade 12, students at post-high school educational institutions, health-care personnel, and international travelers, adequate vaccination for mumps is documentation of 2 doses of live mumps virus-containing vaccine separated by at least 28 days.
Persons who have mumps-specific IgG antibody that is detectable by any commonly used serologic assay are considered to have adequate laboratory evidence of mumps immunity. Persons who have an equivocal serologic test result should be considered susceptible to mumps unless they have other evidence of mumps immunity (Table 3) or subsequent testing indicates mumps immunity.
Safe and effective vaccines for prevention of measles, rubella, and mumps have been available in the United States for more than 40 years. Before availability of vaccines, measles, rubella, and mumps were common diseases in childhood and caused significant morbidity and mortality. As a result of the routine vaccination program, measles and rubella elimination (interruption of endemic transmission chains up to 1 year in length) was achieved in the United States in 2000 and 2004, respectively, and the number of mumps cases has decreased by approximately 99% (48,82,124). In December 2011, an expert panel reviewed available evidence and agreed that the United States has maintained elimination of measles and rubella (50,51). Furthermore, an economic analysis found that the 2-dose MMR vaccination program in the United States resulted in a substantial cost savings (approximately $3.5 billion and $7.6 billion from the direct cost and societal perspectives, respectively) and high benefit-cost ratios: for every dollar spent, the program saves approximately $14 of direct costs and $10 of additional productivity costs (on the basis of estimates using 2001 U.S. dollars) (338).
Despite the success in eliminating and maintaining elimination of endemic transmission of measles and rubella in the United States, the significant decline in mumps morbidity in the United States, and the considerable progress achieved in global measles and rubella control, measles, rubella, CRS, and mumps are still common diseases in many countries. Importations will continue to occur and cause outbreaks in communities that have clusters of unvaccinated persons. Persons who remain unvaccinated put themselves and others in their community, particularly those who cannot be vaccinated, at risk for these diseases and their complications. High levels of population immunity through vaccination are needed to prevent large outbreaks and maintain measles and rubella elimination and low mumps incidence in the United States.
Measles, rubella, and mumps vaccines are recommended for prevention of measles, rubella, and mumps. For prevention of measles and mumps, 1 dose is recommended for preschool-aged children aged ≥12 months and adults not at high risk for exposure and transmission, and 2 doses are recommended for school-aged children in kindergarten through grade 12 and adults at high risk for exposure and transmission (e.g., students attending colleges or other post-high school educational institutions, health-care personnel, and international travelers). For prevention of rubella, 1 dose is recommended for persons aged ≥12 months. Either MMR vaccine or MMRV vaccine can be used to implement the vaccination recommendations for prevention of measles, mumps, and rubella (126). MMR vaccine is indicated for persons aged ≥12 months. MMRV vaccine is licensed for use only in children aged 12 months through 12 years. The minimum interval between the 2 doses of MMR vaccine or MMR vaccine and MMRV vaccine is 28 days, with the first dose administered at age ≥12 months. The minimum interval between 2 doses of MMRV vaccine is 3 months.
ACIP recommends that for the first dose of measles, mumps, rubella, and varicella vaccines at age 12 through 47 months either MMR vaccine and varicella vaccine or MMRV vaccine can be used. Providers who are considering administering MMRV vaccine should discuss the benefits of and risks for both vaccination options with the parents or caregivers. Unless the parent or caregiver expresses a preference for MMRV vaccine, CDC recommends that MMR vaccine and varicella vaccines be administered for the first dose in this age group because of the increased risk for febrile seizures 5 through 12 days after vaccination with MMRV vaccine compared with MMR vaccine among children aged 12 through 23 months (126,298,299).
For the second dose at any age (15 months through 12 years) and the first dose at age 48 months through 12 years, use of MMRV vaccine generally is preferred as opposed to separate injections of its equivalent component vaccines (MMR vaccine and varicella vaccine). Considerations for using separate injections instead of MMRV vaccine should include provider assessment (i.e., the number of injections, vaccine availability, likelihood of improved coverage, likelihood of patient return, and storage and cost considerations), patient preference, and potential adverse events (see ACIP recommendations on use of combination MMRV vaccine) (126).
All eligible children should receive the first dose of MMR vaccine routinely at age 12 through 15 months. Vaccination with MMR vaccine is recommended for all children as soon as possible upon reaching age 12 months.
The second dose of MMR vaccine is recommended routinely for all children aged 4 through 6 years before entering kindergarten or first grade. However, the second dose of MMR vaccine can be administered at an earlier age if the interval between the first and second dose is more than 28 days.
Adults born in 1957 or later should receive at least 1 dose of MMR vaccine unless they have other acceptable evidence of immunity to these three diseases (Table 3). However, persons who received measles vaccine of unknown type, inactivated measles vaccine, or further attenuated measles vaccine accompanied by IG or high-titer measles immune globulin (no longer available in the United States) should be considered unvaccinated and should be revaccinated with 1 or 2 doses of MMR vaccine. Persons vaccinated before 1979 with either killed mumps vaccine or mumps vaccine of unknown type who are at high risk for mumps infection (e.g., persons who are working in a health-care facility) should be considered for revaccination with 2 doses of MMR vaccine.
Adults born before 1957 can be considered to have immunity to measles, rubella (except for women who could become pregnant), and mumps. However, MMR vaccine (1 dose or 2 doses administered at least 28 days apart) can be administered to any person born before 1957 who does not have a contraindication to MMR vaccination.
Adults who might be at increased risk for exposure or transmission of measles, rubella, or mumps and who do not have evidence of immunity should receive special consideration for vaccination. Students attending colleges or other post-high school educational institutions, health-care personnel, and international travelers should receive 2 doses of MMR vaccine.
All students entering school, colleges, universities, technical and vocational schools, and other institutions for post-high school education should receive 2 doses of MMR vaccine (with the first dose administered at age ≥12 months) or have other evidence of measles, rubella, and mumps immunity (Table 3) before enrollment. Students who have already received 2 appropriately spaced doses of MMR vaccine do not need an additional dose when they enter school.
To prevent disease and transmission in health-care settings, health-care institutions should ensure that all persons who work in health-care facilities have documentation of adequate vaccination against measles, rubella, and mumps or other acceptable evidence of immunity to these diseases (Table 3) (6).
Health-Care Personnel Born During or After 1957
Adequate vaccination for health-care personnel born during or after 1957 consists of 2 doses of live measles virus-containing vaccine, 2 doses of live mumps virus-containing vaccine, and at least 1 dose of a live rubella virus-containing vaccine (Table 3). The second dose of live measles virus-containing or mumps virus-containing vaccine should be administered at least 28 days after their first dose. Health-care facilities should use secure, preferably computerized, systems to manage vaccination records for health-care personnel so records can be retrieved easily (6).
Health-Care Personnel Born Before 1957
Although birth before 1957 is considered acceptable evidence of measles, rubella, and mumps immunity, health-care facilities should consider vaccinating unvaccinated personnel born before 1957 who do not have laboratory evidence of measles, rubella, and mumps immunity; laboratory confirmation of disease; or vaccination with 2 appropriately spaced doses of MMR vaccine for measles and mumps and 1 dose of MMR vaccine for rubella. Vaccination recommendations during outbreaks differ from routine recommendations for this group (see section titled Recommendations during Outbreaks of Measles, Rubella, or Mumps).
Serologic Testing of Health-Care Personnel
Prevaccination antibody screening before measles, rubella, or mumps vaccination for health-care personnel who do not have adequate presumptive evidence of immunity is not necessary unless the medical facility considers it cost effective. For health-care personnel who have 2 documented doses of measles- and mumps- containing vaccine and 1 documented dose of rubella-containing vaccine or other acceptable evidence of measles, rubella, and mumps immunity, serologic testing for immunity is not recommended. If health-care personnel who have 2 documented doses of measles- or mumps- containing vaccine are tested serologically and have negative or equivocal titer results for measles or mumps, it is not recommended that they receive an additional dose of MMR vaccine. Such persons should be considered to have acceptable evidence of measles and mumps immunity; retesting is not necessary. Similarly, if health-care personnel (except for women of childbearing age) who have one documented dose of rubella-containing vaccine are tested serologically and have negative or equivocal titer results for rubella, it is not recommended that they receive an additional dose of MMR vaccine. Such persons should be considered to have acceptable evidence of rubella immunity.
International Travelers Aged ≥6 Months
Measles, rubella, and mumps are endemic in many countries and protection against measles, rubella, and mumps is important before international travel. All persons aged ≥6 months who plan to travel or live abroad should ensure that they have acceptable evidence of immunity to measles, rubella, and mumps before travel (Table 3). Travelers aged ≥6 months who do not have acceptable evidence of measles, rubella, and mumps immunity should be vaccinated with MMR vaccine. Before departure from the United States, children aged 6 through 11 months should receive 1 dose of MMR vaccine and children aged ≥12 months and adults should receive 2 doses of MMR vaccine separated by at least 28 days, with the first dose administered at age ≥12 months. Children who received MMR vaccine before age 12 months should be considered potentially susceptible to all three diseases and should be revaccinated with 2 doses of MMR vaccine, the first dose administered when the child is aged 12 through 15 months (12 months if the child remains in an area where disease risk is high) and the second dose at least 28 days later.
Women of Childbearing Age
All women of childbearing age (i.e., adolescent girls and premenopausal adult women), especially those who grew up outside the United States in areas where routine rubella vaccination might not occur, should be vaccinated with 1 dose of MMR vaccine or have other acceptable evidence of rubella immunity. Nonpregnant women of childbearing age who do not have documentation of rubella vaccination, serologic evidence of rubella immunity, or laboratory confirmation of rubella disease should be vaccinated with MMR vaccine. Birth before 1957 is not acceptable evidence of rubella immunity for women who could become pregnant. Women known to be pregnant should not receive MMR vaccine. Upon completion or termination of their pregnancies, women who do not have evidence of rubella immunity should be vaccinated before discharge from the health-care facility. Women should be counseled to avoid becoming pregnant for 28 days after administration of MMR vaccine.
Prenatal serologic screening is indicated for all pregnant women who lack acceptable evidence of rubella immunity (Table 3). Sera sent for screening for immunity should be tested for rubella IgG antibodies only and not for rubella IgM antibodies, unless a suspicion exists of recent rubella exposure (i.e., contact with a person suspected or confirmed to have contracted rubella). Testing for rubella IgM might lead to detection of nonspecific IgM, resulting in a false positive test result and long-persisting IgM results that are difficult to interpret (339).
Household and Close Contacts of Immunocompromised Persons
Immunocompromised persons are at high risk for severe complications if infected with measles. All family and other close contacts of immunocompromised persons aged ≥12 months should receive 2 doses of MMR vaccine unless they have other evidence of measles immunity (Table 3).
Persons with Human Immunodeficiency Virus (HIV) Infection
Vaccination of Persons with HIV Infection Who Do Not Have Current Evidence of Severe Immunosuppression
Two doses of MMR vaccine are recommended for all persons aged ≥12 months with HIV infection who do not have evidence of measles, rubella, and mumps immunity or evidence of severe immunosuppression. Absence of severe immunosuppression is defined as CD4 percentages ≥15% for ≥6 months for persons aged ≤5 years and CD4 percentages ≥15% and CD4 count ≥200 lymphocytes/mm3 for ≥6 months for persons aged >5 years. When only CD4 counts or CD4 percentages are available for those aged >5 years, the assessment of severe immunosuppression can be on the basis of the CD4 values (count or percentage) that are available. When CD4 percentages are not available for those aged ≤5 years, the assessment of severe immunosuppression can be on the basis of age-specific CD4 counts at the time CD4 counts were measured (i.e., absence of severe immunosuppression is defined as ≥6 months above age-specific CD4 count criteria: CD4 count >750 lymphocytes/mm3 while aged ≤12 months and CD4 count ≥500 lymphocytes/mm3 while aged 1 through 5 years).
The first dose of MMR vaccine should be administered at age 12 through 15 months and the second dose at age 4 through 6 years, or as early as 28 days after the first dose. Older children and adults with newly diagnosed HIV infections and without acceptable evidence of measles, rubella, or mumps immunity (Table 3) should complete a 2-dose schedule with MMR vaccine as soon as possible after diagnosis, unless they have evidence of severe immunosuppression (i.e., CD4 percentage <15% [all ages] or CD4 count <200 lymphocytes/mm3 [aged >5 years]). MMRV vaccine has not been studied in persons with HIV infection and should not be substituted for MMR vaccine.
Revaccination of Persons with Perinatal HIV Infection Who Do Not Have Evidence of Severe Immunosuppression
Persons with perinatal HIV infection who were vaccinated with measles-, rubella-, or mumps-containing vaccine before establishment of effective ART should receive 2 appropriately spaced doses of MMR vaccine (i.e., 1 dose now and another dose at least 28 days later) once effective ART has been established unless they have other acceptable current evidence of measles, rubella, and mumps immunity (Table 3). Established effective ART is defined as receiving ART for ≥6 months in combination with CD4 percentages ≥15% for ≥6 months for persons aged ≤5 years and CD4 percentages ≥15% and CD4 count ≥200 lymphocytes/mm3 for ≥6 months for persons aged >5 years. When only CD4 counts or only CD4 percentages are available for those aged >5 years, the assessment of established effective ART can be on the basis of the CD4 values (count or percentage) that are available. When CD4 percentages are not available for those aged ≤5 years, the assessment of established effective ART can be on the basis of age-specific CD4 counts at the time CD4 counts were measured (i.e., established effective ART is defined as receiving ART for ≥6 months in combination with meeting age-specific CD4 count criteria for ≥6 months: CD4 count >750 lymphocytes/mm3 while aged ≤12 months and CD4 count ≥500 lymphocytes/mm3 while aged 1 through 5 years).
During measles, rubella, or mumps outbreaks, efforts should be made to ensure that all persons at risk for exposure and infection are vaccinated or have other acceptable evidence of immunity (Table 3). Evidence of adequate vaccination for school-aged children, college students, and students in other postsecondary educational institutions who are at risk for exposure and infection during measles and mumps outbreaks consists of 2 doses of measles- or mumps-containing vaccine separated by at least 28 days, respectively. If the outbreak affects preschool-aged children or adults with community-wide transmission, a second dose should be considered for children aged 1 through 4 years or adults who have received 1 dose. In addition, during measles outbreaks involving infants aged <12 months with ongoing risk for exposure, infants aged ≥6 months can be vaccinated. During mumps outbreaks involving adults, MMR vaccination should be considered for persons born before 1957 who do not have other evidence of immunity and might be exposed. Adequate vaccination during rubella outbreaks for persons aged ≥12 months consists of 1 dose of rubella-containing vaccine.
CDC guidance for surveillance and outbreak control for measles, rubella, CRS, and mumps can be found in the Manual for the Surveillance of Vaccine-Preventable Diseases (http://www.cdc.gov/vaccines/pubs/surv-manual/index.html).
During an outbreak of measles or mumps, health-care facilities should recommend 2 doses of MMR vaccine at the appropriate interval for unvaccinated health-care personnel regardless of birth year who lack laboratory evidence of measles or mumps immunity or laboratory confirmation of disease. Similarly, during outbreaks of rubella, health-care facilities should recommend 1 dose of MMR vaccine for unvaccinated personnel regardless of birth year who lack laboratory evidence of rubella immunity or laboratory confirmation of infection or disease. Serologic screening before vaccination is not recommended during outbreaks because rapid vaccination is necessary to halt disease transmission (6). If documentation of adequate evidence of immunity has not already been collected, it might be difficult to quickly obtain documentation of immunity for health-care personnel during an outbreak or when an exposure occurs. Therefore, health-care facilities might want to ensure that the measles, rubella, and mumps immunity status of health-care personnel is routinely documented and can be easily accessed.
MMR vaccine, if administered within 72 hours of initial measles exposure, might provide some protection or modify the clinical course of measles (216–219,222). For vaccine eligible persons aged ≥12 months exposed to measles, administration of MMR vaccine is preferable to using IG, if administered within 72 hours of initial exposure. If exposure does not cause infection, postexposure vaccination should induce protection against subsequent exposures. If exposure results in infection, no evidence indicates that administration of MMR vaccine during the presymptomatic or prodromal stage of illness increases the risk for vaccine-associated adverse events. Postexposure MMR vaccination does not prevent or alter the clinical severity of rubella or mumps and is not recommended.
If administered within 6 days of exposure, IG can prevent or modify measles in persons who are nonimmune. IG is not indicated for persons who have received 1 dose of measles-containing vaccine at age ≥12 months, unless they are severely immunocompromised (as defined later in this report in the subsection titled Immunocompromised patients). IG should not be used to control measles outbreaks, but rather to reduce the risk for infection and complications in the person receiving it. IG has not been shown to prevent rubella or mumps infection after exposure and is not recommended for that purpose.
Any nonimmune person exposed to measles who received IG should subsequently receive MMR vaccine, which should be administered no earlier than 6 months after IGIM administration or 8 months after IGIV administration, provided the person is then aged ≥12 months and the vaccine is not otherwise contraindicated.
The recommended dose of IG administered intramuscularly (IGIM) is 0.5 mL/kg of body weight (maximum dose = 15 mL) and the recommended dose of IG given intravenously (IGIV) is 400 mg/kg.
The following patient groups are at risk for severe disease and complications from measles and should receive IG: infants aged <12 months, pregnant women without evidence of measles immunity, and severely immunocompromised persons. IGIM can be administered to other persons who do not have evidence of measles immunity, but priority should be given to persons exposed in settings with intense, prolonged, close contact (e.g., household, daycare, and classroom). For exposed persons without evidence of measles immunity, a rapid IgG antibody test can be used to inform immune status, provided that administration of IG is not delayed.
Infants aged <12 months. Because infants are at higher risk for severe measles and complications, and infants are susceptible to measles if mothers are nonimmune or their maternal antibodies to measles have waned (337), IGIM should be administered to all infants aged <12 months who have been exposed to measles. For infants aged 6 through 11 months, MMR vaccine can be administered in place of IG if administered within 72 hours of exposure.
Pregnant women without evidence of measles immunity. Because pregnant women might be at higher risk for severe measles and complications (20), IGIV should be administered to pregnant women without evidence of measles immunity who have been exposed to measles. IGIV is recommended to administer doses high enough to achieve estimated protective levels of measles antibody titers.
Immunocompromised patients. Severely immunocompromised patients who are exposed to measles should receive IGIV prophylaxis regardless of immunologic or vaccination status because they might not be protected by the vaccine. Severely immunocompromised patients include patients with severe primary immunodeficiency; patients who have received a bone marrow transplant until at least 12 months after finishing all immunosuppressive treatment, or longer in patients who have developed graft-versus-host disease; patients on treatment for ALL within and until at least 6 months after completion of immunosuppressive chemotherapy; and patients with a diagnosis of AIDS or HIV-infected persons with severe immunosuppression defined as CD4 percent <15% (all ages) or CD4 count <200 lymphocytes/mm3 (aged >5 years) and those who have not received MMR vaccine since receiving effective ART. Some experts include HIV-infected persons who lack recent confirmation of immunologic status or measles immunity.
For persons already receiving IGIV therapy, administration of at least 400 mg/kg body weight within 3 weeks before measles exposure should be sufficient to prevent measles infection. For patients receiving subcutaneous immune globulin (IGSC) therapy, administration of at least 200 mg/kg body weight for 2 consecutive weeks before measles exposure should be sufficient.
To maintain measles, rubella, and CRS elimination, and control of mumps in the United States, rapid detection of cases is necessary so that appropriate control measures can be quickly implemented. This is to prevent imported strains of virus from establishing endemic chains of transmission. Pockets of unvaccinated populations can pose a risk to maintaining elimination of measles, rubella, and CRS and control of mumps, because these diseases will continue to be imported into the United States as long as they remain endemic globally.
The key challenges to maintaining measles, rubella, and CRS elimination and control of mumps in the United States are 1) ensuring high routine vaccination coverage which means vaccinating children at age 12 through 15 months with a first dose of MMR vaccine and ensuring that school-aged children receive a second dose of MMR vaccine (for measles and mumps), 2) vaccinating high risk groups such as health-care personnel, international travelers, including infants aged 6 through 11 months, and students at post-high school educational institutions, 3) maintaining awareness of these diseases among health-care personnel and the public, 4) working with U.S. government agencies and international agencies, including WHO, on global measles and rubella mortality reduction and elimination goals, and 5) ensuring that public health departments continue conducting surveillance and initiating prompt public health responses when a suspect case is reported.
This report is based, in part, on contributions by Preeta K. Kutty, MD, and Susan Redd, National Center for Immunization and Respiratory Diseases, and Albert E. Barskey, MPH, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention.
ACIP Membership List As of October 2012
Chair: Jonathan Temte, MD, PhD, University of Wisconsin School of Medicine and Public Health, Madison, Wisconsin.
Executive Secretary: Larry Pickering, MD, National Center for Immunization and Respiratory Diseases, CDC, Atlanta, Georgia.
Members: Nancy Bennett, MD, University of Rochester School of Medicine and Dentistry, Rochester, New York; Joseph Bocchini, Jr., MD, Louisiana State University Health Sciences Center, Shreveport, Louisiana; Douglas Campos-Outcalt, MD, University of Arizona College of Medicine, Phoenix, Arizona; Tamera Coyne-Beasley, MD, University of North Carolina, Chapel Hill, North Carolina; Jeffrey Duchin, MD, University of Washington, Seattle, Washington; Kathleen Harriman, PhD, California Department of Public Health, Richmond, CA; Lee Harrison, MD, University of Pittsburgh, Pittsburgh, Pennsylvania; Renée Jenkins, MD, Howard University School of Medicine, District of Columbia; Ruth Karron, MD, Johns Hopkins Bloomberg School of Public Health, Baltimore, Maryland; Wendy Keitel, MD, Baylor College of Medicine, Houston, Texas; Sara Rosenbaum, JD, Georgetown University, District of Columbia; Lorry Rubin, MD, Steven and Alexandra Cohen Children's Medical Center of New York, New Hyde Park, New York; Mark Sawyer, MD, University of California at San Diego, California; Marietta Vázquez, MD, Yale University School of Medicine, New Haven, Connecticut.
Ex Officio Members: Vito Caserta, MD, MPH, Health Resources and Services Administration, Rockville, Maryland; Jesse Geibe, MD, Department of Defense, CDC, Atlanta, Georgia; Bruce Gellin, MD, National Vaccine Program Office, District of Columba; Richard Gorman, MD, National Institutes of Health, Bethesda, Maryland; Amy Groom, MPH, Indian Health Service, Albuquerque, New Mexico; Mary Beth Hance, Centers for Medicare and Medicaid Services, Baltimore, Maryland; Linda Kinsinger, MD, Department of Veterans Affairs, Durham, North Carolina; Wellington Sun, MD, Food and Drug Administration, Bethesda, Maryland.
Liaison Representatives: American Academy of Family Physicians, Jamie Loehr, MD, Cayuga Family Medicine, Ithaca, New York; American Academy of Pediatrics, Michael Brady, MD, Ohio State University, Columbus, Ohio, David Kimberlin, MD, University of Alabama School of Medicine, Birmingham, Alabama; American Academy of Physician Assistants, Marie-Michèle Léger, MPH, Alexandria, Virginia; American College Health Association, James C. Turner, MD, University of Virginia School of Medicine, Charlottesville, Virginia; American College of Obstetricians and Gynecologists, Laura Riley, MD, Harvard Medical School, Boston, Massachusetts; American College of Physicians, Gregory Poland, MD, Mayo Clinic, Rochester, Minnesota; American College of Physicians, Sandra Fryhofer, MD, Emory University School of Medicine, Atlanta, Georgia; American Geriatrics Society, Kenneth Schmader, MD, Duke University and Durham VA Medical Centers, Durham, North Carolina; America's Health Insurance Plans, Mark Netoskie, MD, CIGNA, Houston, Texas; American Medical Association, Litjen Tan, PhD, Chicago, Illinois; American Nurses Association, Katie Brewer, MSN, Silver Springs, Maryland; American Osteopathic Association, Stanley Grogg, DO, Oklahoma State University-Center for Health Sciences, Tulsa, Oklahoma; American Pharmacists Association, Stephan L. Foster, PharmD, University of Tennessee Health Sciences Center, College of Pharmacy, Memphis, Tennessee; Association of Immunization Managers, Kelly Moore, MD, Tennessee Department of Health, Nashville, Tennessee; Association for Prevention Teaching and Research, W. Paul McKinney, MD, University of Louisville School of Public Health and Information Sciences, Louisville, Kentucky; Association of State and Territorial Health Officials, José Montero, MD, New Hampshire Department of Health and Human Services, Concord, New Hampshire; Biotechnology Industry Organization, Clement Lewin, PhD, Novartis Vaccines and Diagnostics, Cambridge, Massachusetts; Canadian National Advisory Committee on Immunization, Bryna Warshawsky, MDCM, Middlesex-London Health Unit, London, Ontario, Canada; Council of State and Territorial Epidemiologists, Christine Hahn, MD, Idaho Department of Health and Welfare, Boise, Idaho; Department of Health, United Kingdom, David M. Salisbury, MD, London, United Kingdom; Healthcare Infection Control Practices Advisory Committee, Alexis Elward, MD, Washington University School of Medicine, St Louis, Missouri; Infectious Diseases Society of America, Kathleen Neuzil, MD, University of Washington School of Medicine, Seattle, Washington; Infectious Diseases Society of America, Carol Baker, MD, Baylor College of Medicine, Houston, Texas; National Association of County and City Health Officials, Matthew Zahn, MD, Orange County Health Care Agency, Santa Ana, California; National Association of Pediatric Nurse Practitioners, Patricia Stinchfield, MPH, Children's Hospitals and Clinics of Minnesota, St Paul, Minnesota; National Foundation for Infectious Diseases, William Schaffner, MD, Vanderbilt University School of Medicine, Nashville, Tennessee; National Medical Association, Patricia Whitley-Williams, MD, University of Medicine and Dentistry of New Jersey, New Brunswick, New Jersey; National Vaccine Advisory Committee, Walter Orenstein, MD, Emory University School of Medicine, Atlanta, Georgia; Pharmaceutical Research and Manufacturers of America, Damian A. Braga, Swiftwater, Pennsylvania; Society for Adolescent Health and Medicine, Amy Middleman, MD, Baylor College of Medicine, Houston, Texas; Society for Healthcare Epidemiology of America, Harry Keyserling, MD, Emory University School of Medicine, Atlanta, Georgia.
ACIP Measles, Rubella and Mumps Work Group
Work Group Chair: Jonathan Temte, MD, PhD, University of Wisconsin School of Medicine and Public Health, Madison, Wisconsin (ACIP).
Work Group Members: Tamera Coyne-Beasley, MD, University of North Carolina, Chapel Hill, North Carolina (ACIP); Amy Bashforth,* Ohio Department of Health, Columbus, Ohio; Judy Beeler, MD, U.S. Food and Drug Administration, Bethesda, MD; Kathryn M. Edwards, MD, Vanderbilt University, Nashville, TN; Hayley Gans, MD, Stanford University, Stanford, CA; Samuel L. Katz, MD, Duke University, Durham, North Carolina; Bonnie Maldonado, MD, Stanford University, Stanford, CA; Elizabeth Rosenblum, MD, University of California San Diego Medical Center, San Diego, CA; Marina I. Salvadori, MD, Children's Hospital of Western Ontario, London, Ontario; Mack Sewell, DrPH, MS, Wyoming Department of Workforce Services, Cheyenne, Wyoming; George Siberry, MD, MPH, National Institutes of Health, Bethesda, Maryland; John Talarico,† DO, MPH, California Department of Public Health, Richmond, CA; James C. Turner, MD, University of Virginia, Charlottesville, Virginia.
Work Group Contributors (CDC): William Atkinson, MD, MPH; William Bellini, PhD; Ken Dominguez, MD, MPH; Carole Hickman, PhD; Joseph Icenogle, PhD; Zanie Leroy, MD; Mark Papania, MD, MPH; Amy Parker Fiebelkorn, MSN, MPH; Paul Rota, PhD; Jane Seward, MBBS, MPH; Raymond Strikas, MD, MPH; Gregory Wallace, MD, MS, MPH; Atlanta, Georgia.
Work Group Secretariat (CDC): Huong McLean, PhD, MPH.
* A list of the work group appears on page 34.
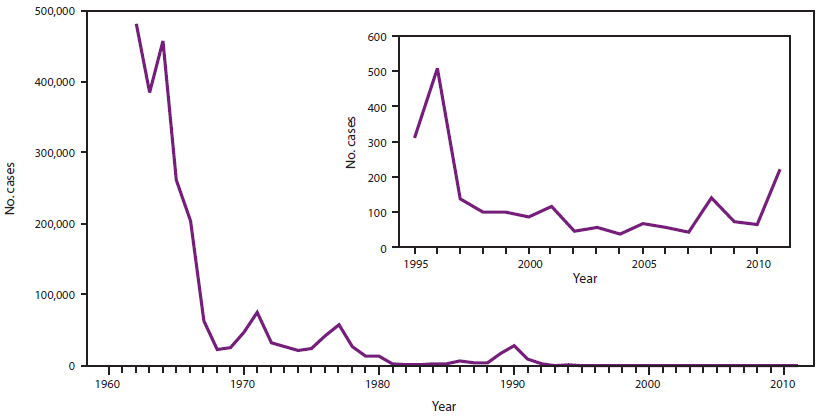
Source: Measles data provided were reported voluntarily to CDC from state health departments.
Alternate Text: This figure provides the number of measles cases in the United States from 1962 through 2011. After the introduction of the 1-dose measles vaccination program, the number of reported measles cases decreased during the late 1960s and early 1970s to approximately 22,000-75,000 cases per year.
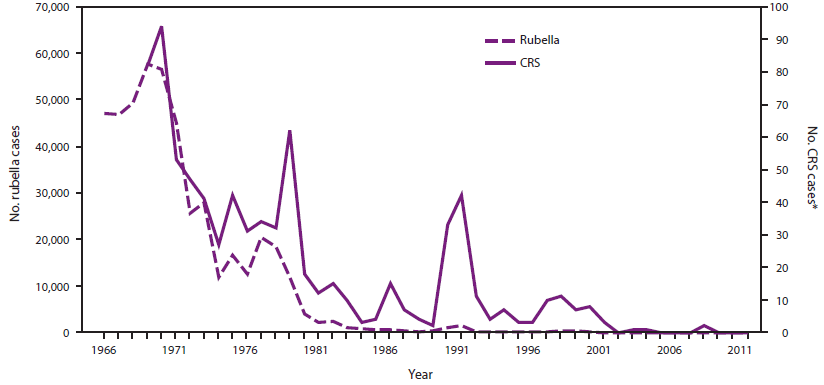
Source: Rubella and CRS data provided were reported voluntarily to CDC from state health departments.
* By year of birth.
Source: Mumps data provided were reported voluntarily to CDC from state health departments.
Alternate Text: This figure provides an overview of the number of rubella cases shown with the jagged line and number of CRS cases shown with the solid line since 1966. After licensure and recommendation for use in 1969, the number of rubella and CRS cases declined dramatically. However, incidence increased in the late 1970s and early 1990s, as a result of outbreaks in unvaccinated populations.
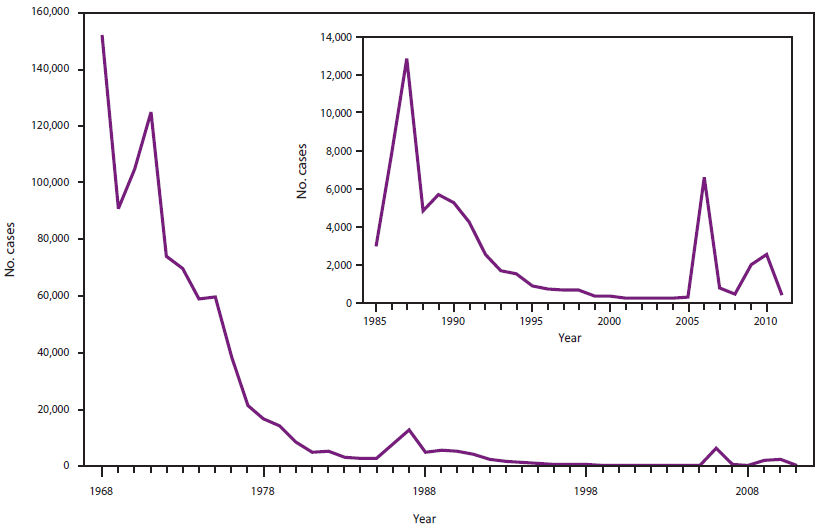
Alternate Text: This figure provides the number of mumps cases in the United States from 1968 through 2011. Reported cases of mumps decreased steadily after the introduction of live mumps vaccine in 1967 and the recommendation in 1977 for routine vaccination.
* Served through May 2012.
† Served from June 2012 through October 2012.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of Health and Human Services.
References to non-CDC sites on the Internet are provided as a service to MMWR readers and do not constitute or imply endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content of pages found at these sites. URL addresses listed in MMWR were current as of the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents. This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.