Heat Stress Illness Hospitalizations — Environmental Public Health Tracking Program, 20 States, 2001–2010
Corresponding author: Ekta Choudhary, Division of Environmental Hazards and Health Effects, National Center for Environmental Health. Telephone: 770-488-3825; E-mail: echoudhary@cdc.gov.
Abstract
Problem/Condition: Heat stress illness (HSI), also known as heat-related illness, comprises mild heat edema, heat syncope, heat cramps, heat exhaustion (the most common type of HSI), and heat stroke (the most severe form). CDC's Environmental Public Health Tracking Program receives annual hospitalization discharge data from 23 states that are used to assess and monitor trends of HSI hospitalization over time.
Reporting Period: May–September, 2001–2010.
Description of System: The Environmental Public Health Tracking Program is a comprehensive surveillance system implemented in 25 states and one city health department. The core of the system is the Tracking Network, which collects data on environmental hazards, health effects, exposures, and population. The Tracking Network provides nationally consistent environmental and health outcome data that enable federal, state, and local public health agencies to assess trends, explore associations, and generate hypotheses using these data. For HSI surveillance, the Tracking Network uses state-based hospital discharge data.
Results: During 2001–2010, approximately 28,000 HSI hospitalizations occurred in 20 states participating in the Tracking Program. Data from three states were not included in this report because of missing data for ≥3 years. Two states joined the Tracking Program after the study period and also are not included in this report. The majority of HSI hospitalizations occurred among males and persons aged ≥65 years. The highest rates of hospitalizations were in the Midwest and the South. During this period, an overall 2%–5% increase in the rate of HSI hospitalizations occurred in all 20 states compared with the 2001 rate. The correlation between the average number of HSI hospitalizations and the average monthly maximum temperature/heat index was statistically significant (at p<0.0001) in all 20 states.
Interpretation: Consistent with previous studies, age and sex were identified as major risk factors for HSI hospitalizations. Certain Tracking states that experienced high temperatures during summer months showed an increase in rate of HSI hospitalizations over the 10-year study period.
Public Health Action: HSIs are preventable and an important focus of public health interventions at state and local health departments. Federal, state, and local public health agencies can use data on HSI hospitalizations for surveillance purposes to estimate trends over time and to design targeted intervention to reduce heat stress morbidity among at-risk populations.
Introduction
All persons, regardless of age, sex, or health status, are at risk for heat stress illness (HSI), also known as heat-related illness (1). The body's physiologic mechanisms maintain a person's core body temperature (i.e., the operating temperature of vital organs in the head or trunk) in a narrow optimal range around 98.6° F (37° C) (1). When a person's core body temperature rises, the body's immediate physiologic response is to sweat and circulate blood closer to the skin's surface so as to increase cooling (2). If heat exposure exceeds the body's physiologic capacity to cool, and if the person's core body temperature then rises, a range of heat stress symptoms and conditions can develop.
HSI ranges from mild heat cramps, heat exhaustion, and heat syncope to the most severe condition, heat stroke (1). HSI can manifest in multiple clinical outcomes, and persons with chronic health conditions (e.g., cardiovascular disease, diabetes, or obesity) are more susceptible to the effects of heat than persons without such conditions (3). For these reasons, HSI might not always be listed as the primary diagnosis in the discharge data collected by local hospitals. Despite this limitation, discharge data from local hospitals can be used to monitor the prevalence of HSI and examine heat stress morbidity (4–6).
Background
The relationship between extreme temperatures, increased HSI, and deaths is well established (3,7). Increases in the rates of HSI hospitalizations are one of the many potential impacts of extreme heat (4,8,9). Monitoring heat-related hospitalizations can help document changes in the burden of HSI over place and time, identify and monitor vulnerable areas, and evaluate the effectiveness of local climate-adaptation strategies.
Hospital discharge data are state-based administrative data created for hospital billing and payment purposes. Information on patient demographics, diagnoses, procedures performed, and sources of payment (including self-pay and uninsured) is collected on all patients discharged from acute-care hospitals within a state (6). Since approximately 1990, state hospital discharge data systems have provided information to researchers, policy makers, providers, and consumers to improve health-care cost, quality, and health-care access (10). As the only source of hospital use data that includes all patients and all payers from in a state, hospital discharge data support multiple community and national health information initiatives (10).
This report analyzes data on HSI hospitalizations from CDC's Environmental Public Health Tracking Program for 2001–2010 to summarize the incidence of HSI and examine the trend in the rate of HSI hospitalizations by age, sex, county, and state. The findings in this report can be used by federal, state, and local public health professionals for surveillance purposes to estimate trends over time and to design targeted intervention to reduce heat stress morbidity among at-risk populations.
Methods
Data Source
CDC's Environmental Public Health Tracking Program was established in 2002 and has been implemented in 25 states and one large city health department* (11). The core of this program is the Tracking Network, which includes information on environmental hazards, health effects, exposures, and population data that are received primarily from states and national sources. All of the Tracking Network participants develop local tracking networks, whose efforts feed into the National Tracking Network. Partnerships between federal, state, and local public and environmental health agencies have helped the Tracking Network develop and adopt nationally consistent indicators and measures. Data are presented as measures and organized by indicator for each content area. A content area might focus on health, exposure, the environment, or the intersection of health and the environment (11). The Tracking Network allows users to view data in maps, tables, and charts; search and view metadata; and find information about their community's health and environment (11).
Data Collection and Processing
The Tracking Network receives hospitalization discharge data from 25 funded states. Of these 25 states, 23 states† have a mandate to collect hospital discharge data at the state level, and two states (Michigan and Colorado) collect data voluntarily (Figure 1) (12). For this report, data were used from 20 states to examine trends of HSI. Data from two new Tracking Network grantee states (Michigan and Kentucky) were not included because these states received funding in October 2014, after the study period covered in this report. Data from three other states (Colorado, Maryland, and New Hampshire) were not used because ≥3 years of data were missing.
Tracking Network states submit de-identified county-level hospitalization data for HSI to the National Tracking Network annually. HSI hospitalizations are submitted as monthly aggregates for the summer months (May–September) per year to the Tracking Network. These data then are used to calculate annual state level estimates (number, crude rate, and age-adjusted rate), and these estimates are displayed in the Tracking Network's Internet web portal (available at http://ephtracking.cdc.gov/showHome.action).
Data collection begins at in-patient hospitals, which create and maintain patient transaction information. Hospitals submit hospitalization discharge data, usually quarterly, to state data stewards, which can be either public organizations (e.g., a part of the state government) or a delegated authority (e.g., a hospital association or private entity). After validating and finalizing the hospitalization discharge data, state data stewards transfer the data to state tracking programs, which submit de-identified hospitalization discharge data to the Tracking Network annually. The Tracking program has developed standardized guidelines for preparing and submitting hospitalization data that all states are required to follow. Once data are received by the Tracking Program, all hospitalization data are processed to create nationally consistent data and measures that become available to stakeholders, including the public, via a web-based query system (13).
Case Definition
HSI might not always be listed as the primary diagnosis in the discharge data collected by local hospitals. For all possible cases of HSI to be captured, all cases for which the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) code for HSI is listed explicitly as either the primary diagnosis or as any other diagnosis must be included. HSI hospitalization was defined as any illness requiring hospital admission (i.e., in-patient hospital stay for ≥23 hours) for which a primary or other diagnosis ICD-9-CM code in the range of 992.0–992.9 or cause-of-injury code E900.0 or E900, excluding cases with a code of E900.1 (exposure to a man-made source of heat), was recorded. All cases that met the case definition and occurred during May–September of each year during 2001–2010 were included in the analyses.
Analytic Methods
The total number of HSI cases in 20 states for the 10-year study period 2001–2010 was measured, and crude and age-adjusted rates of HSI hospitalization per 100,000 population were calculated at the state and county level. Correlations between number of monthly HSI hospitalizations and average monthly maximum temperature at the county level were examined for all 20 states. Changes in the rate of HSI hospitalizations over the 10-year study period also were examined.
Modeled meteorology data from the North American Land Data Assimilation System were processed by the Tracking Program to create indicators for use in extreme heat surveillance and research. Tracking Network users have access to county-level daily heat metrics data (e.g., daily maximum temperature and heat index) for 1979–2011. Average monthly heat metrics were generated for daily (24-hour) maximum temperature, and heat index was generated from daily data (14). County-level data were linked with hospitalization data to explore the relationship between hospital discharge data and temperature.
Tracking Network states provided county-level monthly aggregates for HSI cases for each year, which CDC used to calculate county- and state-level yearly totals. Crude rates of HSI per 100,000 population were calculated by using midyear resident population from the U.S. Census Bureau (15,16); annual age-adjusted rates were calculated by the direct method using the 2000 U.S. Standard Population, divided into 18 age groups (17). The 10-year average crude rate per 100,000 population was calculated by using the 10-year average number of HSI hospitalizations as the numerator and the 10-year average population as the denominator from 20 states. Spearman rank correlation was used to examine the correlation between monthly number of HSI cases, the average monthly maximum temperature, and the average monthly heat index; statistical significance was determined as p<0.05. Poisson log-linear regression analyses were used to examine the trend of heat stress rates over time, with 2001 data used as the baseline.
The incident rate ratio (IRR) of HSI hospitalizations over time was calculated. Rates and IRRs were calculated with a 95% confidence interval; statistical significance was determined as p<0.05. The expected count of HSI hospitalizations (z) per year (t) in a state (s) was modeled as follows:

where Pt is the population of the state in year t and zt is the number of HSI hospitalizations. All analyses were performed by using SAS version 9.3, and maps were created by using ESRI ArcGIS version 10.1.
Results
Demographics
During 2001–2010, a total of 28,133 HSI hospitalizations were reported in 20 Tracking Network states (Table 1). A majority of the cases were in males (69.2%) and a plurality were in persons aged ≥65 years (42.3%). During the study period, the highest number of HSI hospitalizations (n = 4,022) was reported in 2006, and the lowest number (n = 1,737) was reported in 2004. Similarly, the highest crude and age-adjusted rates per 100,000 population per year (crude rate: 2.7; age-adjusted rate: 2.5) were observed in 2006, and the lowest rates (crude rate: 1.7; age-adjusted rate: 1.1) were observed in 2004.
Rate of HSI Hospitalizations
Among the 20 Tracking Network states over the 10-year period, the highest number of HSI cases (n = 5,385) was reported in California, and the lowest number of cases (n = 37) was reported in Vermont. The crude and age-adjusted rate of HSI hospitalizations per 100,000 population in 20 Tracking Network states from 2001 to 2010 are reported (Tables 2 and 3). Five states (Florida, Louisiana, Kansas, Missouri, and South Carolina) had the highest crude and age-adjusted rate of HSI per 100,000 population per year for all 10 study years (Figures 2 and 3).
The 10-year average crude rate of HSI hospitalizations at the county level in 20 Tracking Network states is reported (Figure 4). The five counties with the highest 10-year average crude rate of HSI hospitalizations per 100,000 population were Lane County, Kansas (32.2); Gove County, Kansas (31.8); Pemiscot County, Missouri (28.3); Clark County, Kansas (26.2); and Madison County, Louisiana (24.5). The 10-year average age-adjusted rate of HSI hospitalizations at the county level is reported for 20 Tracking Network states (Figure 5). Similar to the crude rate, the five counties with the highest 10-year average age-adjusted rate of HSI hospitalizations per 100,000 population were Gove County, Kansas (33.8); Pemiscot County, Missouri (27.9); Madison County, Louisiana (25.1); Lane County, Kansas (24.9); and Morton County, Kansas (20.4).
Trend Analysis
Trend analysis using Poisson regression showed statistically significant (p<0.05) changes in the rate of HSI hospitalizations in 13 states (Table 4). In eight states (California, Connecticut, Florida, Louisiana, Missouri, New Mexico, South Carolina, and Washington), the increase in the rate of hospitalization ranged from 2% to 6% over the 10-year period, using the 2001 rate as the baseline. Kansas was among the five states with the highest crude and age-adjusted rates of HSI hospitalization, but a statistically significant increase in the rate of HSI hospitalizations over the 10-year period was not observed (p<0.05). Alternatively, a decrease (range: 5%–12%) was observed in the rate of heat stress hospitalizations in five states (Iowa, Maine, Massachusetts, New York, and Wisconsin) (Table 4).
Correlation Between Temperature and Heat Stress Illness
The correlation between the 10-year monthly average number of HSI hospitalizations at the state level and the 10-year monthly average maximum temperature at the county level was examined in 20 Tracking Network states (Table 5). In all 20 states, a statistically significant correlation was observed between monthly average number of HSI hospitalizations and average monthly maximum temperature. The strongest correlation was observed in Massachusetts (ρ[700] = 0.54; p<0.0001) and the weakest correlation was seen in Florida (ρ[3350] = 0.07, p<0.0001). The six northeastern states showed the strongest correlation between monthly average number of HSI hospitalizations and average monthly maximum temperature: Massachusetts (ρ[700] = 0.54; p<0.0001), New Jersey (ρ[1050] = 0.49; p<0.0001), Connecticut (ρ[400] = 0.44; p<0.0001), New York (ρ[3100] = 0.41; p<0.0001), and Pennsylvania (ρ[3350] = 0.39; p<0.0001). Similarly, a correlation was observed between the monthly average number of HSI hospitalizations and the monthly average heat index (Table 6). The strongest correlation was seen in Massachusetts (ρ[700] = 0.55; p<0.0001), and the lowest correlation was observed in Vermont (ρ[700] = 0.17; p<0.0001). The Northeastern states showed the strongest correlation between the average number of HSI hospitalizations and the monthly average heat index: Massachusetts (ρ[700] = 0.55; p<0.0001), New Jersey (ρ[1050] = 0.52; p<0.0001), Connecticut (ρ[400] = 0.46; p<0.0001), New York (ρ[3100] = 0.42; p<0.0001) and Pennsylvania (ρ[3350] = 0.41; p<0.0001).
Discussion
HSIs are generally preventable and are an important focus for public health interventions at state and local health agencies. The findings in this report indicate that Tracking Network states in the South and the Midwest had the highest rate of HSI over the 10-year period. A small increase was observed in the rate of HSI hospitalizations in a majority of the Tracking Network states, but a slight decrease occurred in others (mainly in the northern states). For states in the Northeast, a relatively strong positive correlation was found between the number of HSI hospitalizations and the average monthly maximum temperature/heat index.
Previous studies have identified sex as a risk factor for HSI. Men are more likely than women to work outdoors and seek medical help for HSI (3,7). Consistent with these studies, the findings in this report demonstrate that approximately 70% of the HSI cases occurred among males. Similarly, rates of HSI hospitalization over the 10-year period were also higher among males. Similar findings were reported in studies that focused on occupational and recreational heat exposures (3,18,19).
Previous studies also have identified age as a risk factor for HSI (4,5,7,9,20). The findings in this report indicate that the majority (83.1%) of HSI hospitalizations occurred among persons aged ≥35 years, and especially among persons aged ≥65 years (approximately 43.0%). Data recorded during a 2006 California heat wave also indicated that 52% of the excess number of HSI hospitalizations that occurred during heat waves were among persons aged ≥65 years (4). Another study conducted in Australia found that 39% of HSI hospitalization occurred among persons aged ≥65 years (9). The findings in this report also identified persons aged ≥65 years as being at higher risk for HSI than persons aged <65 years.
Midwestern and Southern states usually experience higher temperatures in summer months compared with Northern states. Exposure to extreme temperatures has been associated with both mortality and morbidity (21). Hospital discharge data and temperature data in 20 Tracking Network states showed that the highest numbers of HSI hospitalizations occurred in the Midwestern and Southern states. The highest rate of HSI hospitalizations and an increasing trend in hospitalizations also were observed in these states. Similarly, the counties with highest rates of HSI hospitalizations were also in the Midwestern and Southern states. Among the 20 Tracking Network states, the number and rates of HSI were highest in Missouri. An increase in HSI hospitalization trend also was observed in Missouri over the 10-year study period. Missouri is the only state in which HSI that is diagnosed by a physician is a reportable disease,§ which possibly contributed to increased reporting of HSI hospitalizations in the state (22,23).
Temperature data from the National Oceanic and Atmospheric Administration's National Climatic Data Center indicate that in all 50 states, average monthly temperatures in the summer months (May–September) during 2001–2010 were higher compared with the same months during 1981–2000 (8,24,25,26). Most states experienced very high temperatures in 2006 and 2007 (23). The findings in this report indicate that the rate of HSI hospitalizations in 20 Tracking Network states was highest in 2006. A previous study reported the impact of the 2006 heat wave on HSI hospitalizations and emergency department visits in California (4). Poisson regression analysis confirms that an annual increase in the rate of HSI hospitalizations occurred. The increasing trend of HSI hospitalizations during 2001–2010 and the association with temperature data show the effects of increased monthly temperatures over time. Previous studies have observed similar trends in heat-related mortality and morbidity (3,7,25,26).
The findings provided in this report demonstrate that a substantial number of heat stress hospitalizations occurred in the Midwest and the South. Moreover, a strong correlation was observed between temperature and an increase in the number of hospitalizations in the Northeast. Persons in places with high temperatures might adapt to high temperatures and also might limit their exposure to higher temperatures (3,5,21). Unlike states in the Midwest and the South, the Northeast does not experience persistent high temperatures, and the populations in these states therefore might be less acclimatized to the high temperatures that can result in HSI and subsequent hospitalizations.
Limitations
The findings provided in this report are subject to at least seven limitations. First, periods of extreme heat frequently are associated with increases in hospital visits and admissions for many causes. Data collected by the Tracking Network might not capture the full spectrum of heat stress, especially if exposure to excess heat is not documented explicitly in the patient records. Second, hospitalization data include transfers between hospitals for the same person for the same heat stress event. Therefore, variations in the percentage of transfers or re-admissions for the same heat stress event might vary by geographical area and impact rates. Third, some of the Tracking states do not have reciprocal reporting agreements with neighboring states; therefore, statewide measures and measures for geographic areas (e.g., counties) bordering other states might be underestimated because of health care use patterns. Fourth, hospitalization data collected by Tracking Network states excludes data from Veterans Affairs Medical Centers, Indian Health Services, and institutionalized (e.g., prison) populations, which might result in some underreporting of HSI hospitalizations. Fifth, variations in medical practice patterns and payment mechanisms at the state level might affect diagnostic coding and treatment decisions by health-care providers to hospitalized patients. Sixth, in addition, patients might be exposed to environmental triggers in multiple locations, but hospital discharge geographic information is limited to residence. Finally, because the data capture hospital discharges (rather than admissions), and because cases are identified on the basis of the date of admission, patients admitted toward the end of the year and discharged the following year will be omitted from the current year data set. Also, a very small number of cases at the county level might result in an unstable rate at the county and state levels.
Conclusion
Increases in summer temperatures are associated with an increase in HSI (4,25,27). A comparison of HSI hospitalizations at the state and county level indicates that the Midwestern and Southern states had the highest number of HSI hospitalizations; however, a strong correlation between temperature and HSI hospitalizations also was observed in the Northeastern states. State and local health departments are interested in preventing health impacts associated with extreme heat, especially among vulnerable populations (27,28).
To gauge the public health burden to extreme heat, researchers need to understand the extent of HSI exposure and identify risk factors. HSI hospitalization surveillance provides an important measure of heat stress surveillance. In addition, state and local health departments may find it beneficial to track heat stress morbidity over time to understand and evaluate the impact of public health interventions. This study highlights the use of hospital discharge data, an existing data source in most states, for HSI surveillance. Federal, state, and local health department can utilize this invaluable data source to examine burden of HSI during summer months.
HSIs are preventable by avoiding exposure to high temperatures. State and local health agencies can work collaboratively to inform the general population about extreme weather conditions in advance (11). They can increase awareness on how persons can limit their exposure to extreme temperatures and information on any resources available to the public. State health departments could open cooling centers or encourage use of public facilities with air conditioning to mitigate extreme heat exposure. For example, one of the Tracking Network states used the hospitalizations and emergency department visits data along with temperature data to show the burden of HSI. On the basis of this evidence, local public health professionals and decision-makers decided to open cooling centers as part of the local heat alert response. This example indicates how surveillance for heat stress illness can help identify local patterns of vulnerability to best target an at-risk population, devise public health interventions, and implement emergency response activities.
Acknowledgments
This report is based, in part, on data provided by Tracking partners from California, Connecticut, Florida, Iowa, Kansas, Louisiana, Maine, Massachusetts, Minnesota, Missouri, New Jersey, New Mexico, New York, New York City, Oregon, Pennsylvania, South Carolina, Utah, Vermont, Washington, and Wisconsin. Maps were generated by CDC's Geospatial Research, Analysis, and Services Program (GRASP).
References
- Lugo-Amador NM, Rothenhaus T, Moyer P. Heat-related illness. Emerg Med Clin North Am 2004;22:315–27.
- Blum LN, Bresolin LB, Williams MA. From the AMA Council on Scientific Affairs. Heat-related illness during extreme weather emergencies. JAMA 1998;279:1514.
- Noe RS, Choudhary E, Cheng-Dobson LJ, Wolkin AF, Newman SB. Exertional heat-related illnesses at the Grand Canyon National Park, 2004–2009. Wilderness Environ Med 2013;24:422–8.
- Knowlton K, Rotkin-Ellman M, King G, et al. The 2006 California heat wave: impacts on hospitalizations and emergency department visits. Environ Health Perspect 2009;117:61–7.
- Zhang Y, Nitschke M, Bi P. Risk factors for direct heat-related hospitalization during the 2009 Adelaide heatwave: a case crossover study. Sci Total Environ 2013;442:1–5.
- Schoenman J, Sutton J, Kintala S, Love D, Maw R. The value of hospital discharge database. Salt Lake City, UT: NORC at University of Chicago; 2005.
- Pillai S, Noe R, Murphy M, et al. Heat illness: predictors of hospital admissions among emergency department visits—Georgia, 2002–2008. J Community Health 2013;2013:1–9.
- Karl TR, Trenberth KE. Modern global climate change. Science 2003;302:1719–23.
- Beggs PJ, Vaneckova P. Admission to hospital for effects of heat and light: NSW, 1993–94 to 2003–04. N S W Public Health Bull 2008;19:132–7.
- Love D, Rudolph B, Shah GH. Lessons learned in using hospital discharge data for state and national public health surveillance: implications for Centers for Disease Control and Prevention tracking program. J Public Health Manag Pract 2008;14:533–42.
- CDC. National Environmental Public Health Tracking Network. Atlanta, GA: US Department of Health and Human Services, CDC; 2013. Available at http://ephtracking.cdc.gov/showHome.action.
- CDC. Environmental Public Health Tracking Network. Background. Atlanta, GA: US Department of Health and Human Services, CDC; 2013. Available at http://www.cdc.gov/nceh/tracking/background.htm.
- CDC. National Environmental Public Health Tracking Network. Data re-release plan. Version 2.5. Atlanta, GA: US Department of Health and Human Services, CDC; 2008. Available at http://ephtracking.cdc.gov/docs/Tracking_Re-Release_Plan_v2.5.pdf.
- Rothfusz L. The Heat Index "Equation" (or, more than you wanted to know about Heat Index). Fort Worth, TX: Scientific Services Division, NWS Southern Region HQ; 1990. Available at http://www.srh.noaa.gov/images/ffc/pdf/ta_htindx.pdf.
- CDC, National Center for Health Statistics, National Vital Statistics System. US census populations with bridged race categories. Hyattsville, MD: US Department of Health and Human Services, CDC, National Center for Health Statistics; 2010. Available at http://www.cdc.gov/nchs/nvss/bridged_race.htm.
- US Census Bureau. 2010 census. Washington, DC: US Census Bureau; 2012. Available at http://www.census.gov/2010census/data.
- Klein RJ, Schoenborn CA. Age adjustment using the 2000 projected U.S. population. Healthy People Statistical Notes, no. 20. Hyattsville, Maryland: US Department of Health and Human Services, CDC, National Center for Health Statistics; 2001.
- Rhea S, Ising A, Fleischauer A, Deyneka L, Vaughan-Batten H, Waller A. Using near real-time morbidity data to identify heat-related illness prevention strategies in North Carolina. J Community Health 2012;37:495–500.
- McGeehin MA, Mirabelli M. The potential impacts of climate variability and change on temperature-related morbidity and mortality in the United States. Environ Health Perspect 2001;109(Suppl 2):185–9.
- Anderson GB, Dominici F, Wang Y, McCormack MC, Bell ML, Peng RD. Heat-related emergency hospitalizations for respiratory diseases in the medicare population. Am J Respir Crit Care Med 2013;187:1098–103.
- O'Neill MS, Ebi KL. Temperature extremes and health: impacts of climate variability and change in the United States. J Occup Environ Med 2009;51:13–25.
- Kilbourne EM. The spectrum of illness during heat waves. Am J Prev Med 1999;16:359–60.
- Kilbourne EM, Choi K, Jones TS, Thacker SB. Risk factors for heatstroke: a case-control study. JAMA 1982;247:3332–6.
- National Oceanic and Atmospheric Administration, National Climatic Data Center. Climate at a glance. Washington, DC: National Oceanic and Atmospheric Administration; 2014. Available at http://www.ncdc.noaa.gov/cag/time-series/us/110/00/tmp/5/09/2001-2010?base_prd=true&firstbaseyear=1981&lastbaseyear=2000.
- CDC. Heat illness and deaths—New York City, 2000–2011. MMWR Morb Mortal Wekly Rep 2013;62:617–21.
- Lippmann SJ, Fuhrmann CM, Waller AE, Richardson DB. Ambient temperature and emergency department visits for heat-related illness in North Carolina, 2007–2008. Environ Res 2013;124:35–42.
- O'Neill MS, Carter R, Kish JK, et al. Preventing heat-related morbidity and mortality: New approaches in a changing climate. Maturitas 2009;6:98–103.
- Alberini A, Gans W, Alhassan M. Individual and public-program adaptation: coping with heat waves in five cities in Canada. Int J Environ Res Public Health 2011;8:4679–701.
* California, Colorado, Connecticut, Florida, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Missouri, New Hampshire, New Jersey, New Mexico, New York City, New York, Oregon, Pennsylvania, South Carolina, Utah, Vermont, Washington, and Wisconsin.
† California, Connecticut, Florida, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Minnesota, Missouri, New Hampshire, New Jersey, New Mexico, New York (includes New York City), Oregon, Pennsylvania, South Carolina, Utah, Vermont, Washington, and Wisconsin.
§ Rules of Department of Health and Senior Services Division 20—Division of Community and Public Health Chapter 20—Communicable Diseases (2008).
FIGURE 1. Hospitalization discharge data collection status — United States, 2008
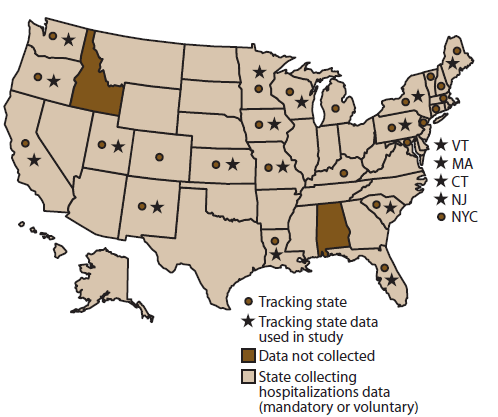
Source: Love D, Rudolph B, Shah GH. Lessons learned in using hospital discharge data for state and national public health surveillance: implications for Centers for Disease Control and Prevention tracking program. J Public Health Manag Pract 2008;14:533–42.
Alternate Text: The figure shows a map of the United States indicating which states that participate in the Environmental Public Health Tracking Program collect hospitalization discharge data.
FIGURE 2. Tracking Network states with the highest crude rate of heat stress illness hospitalizations per 100,000 population — Environmental Public Health Tracking Program, 20 states, 2001–2010
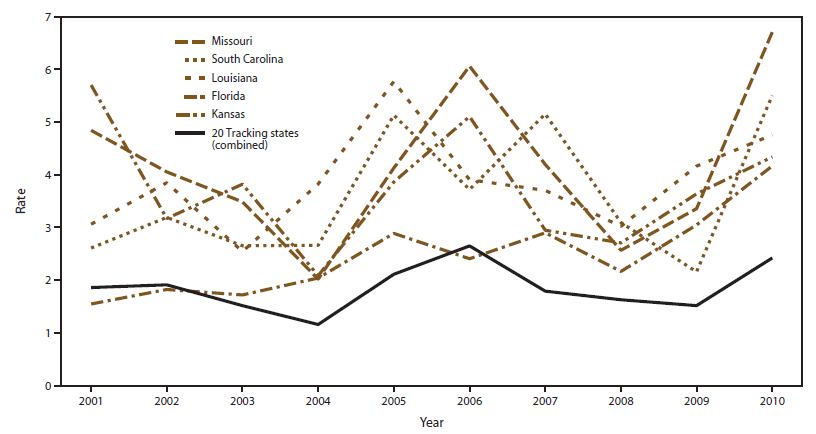
Alternate Text:The figure shows the Environmental Public Health Tracking Network states with the highest crude rates of heat stress illness hospitalizations per 100,000 population during 2001-2010 compared with the overall rate for the 20 states that provided data on heat stress illness hospitalization used in this report. The states with the highest crude rates of heat stress illness hospitalizations were Florida, Louisiana, Kansas, Missouri, and South Carolina.
FIGURE 3. Tracking Network states with the highest age-adjusted rates of heat stress illness hospitalizations per 100,000 population — Environmental Public Health Tracking Program, 20 States, 2001–2010
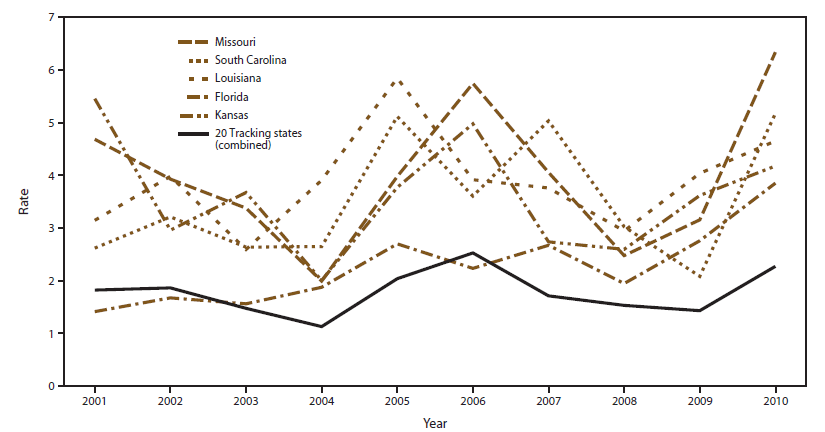
Alternate Text:The figure shows the Environmental Public Health Tracking Network states with the highest age-adjusted rates of heat stress illness hospitalizations per 100,000 population during, 2001-2010 compared with the overall rate for the 23 states that provided age-adjusted data used in this report. The states with the highest age-adjusted rates of heat stress illness hospitalizations were Florida, Louisiana, Kansas, Missouri, and South Carolina.
FIGURE 4. Ten-year average crude rate of heat stress illness hospitalizations per 100,000 population, by county — Environmental Public Health Tracking Network, 20 states, 2001–2010
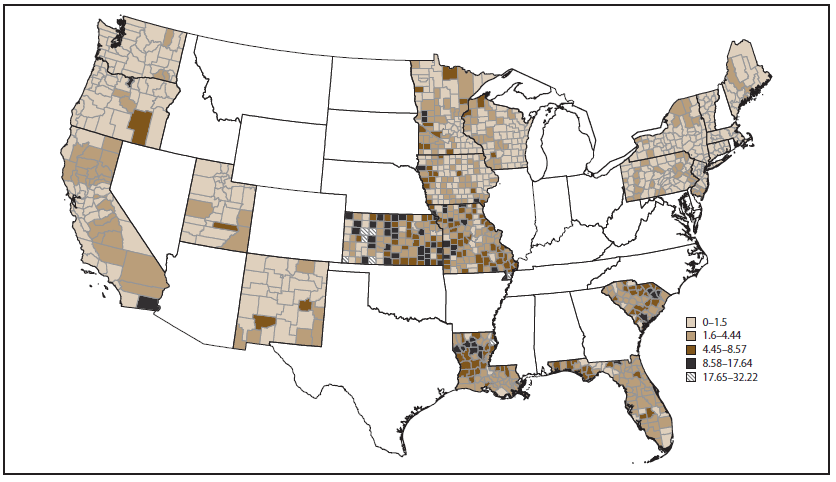
Alternate Text:The figure shows a map of the United States indicating the average crude rate of heat stress illness hospitalizations per 100,000 population, by county, for 20 states that participated in the Environmental Public Health Tracking Network during 2001-2010.
FIGURE 5. Ten-year average age-adjusted rate of heat stress illness hospitalizations per 100,000 population, by county — Environmental Public Health Tracking Network, 20 states, 2001–2010
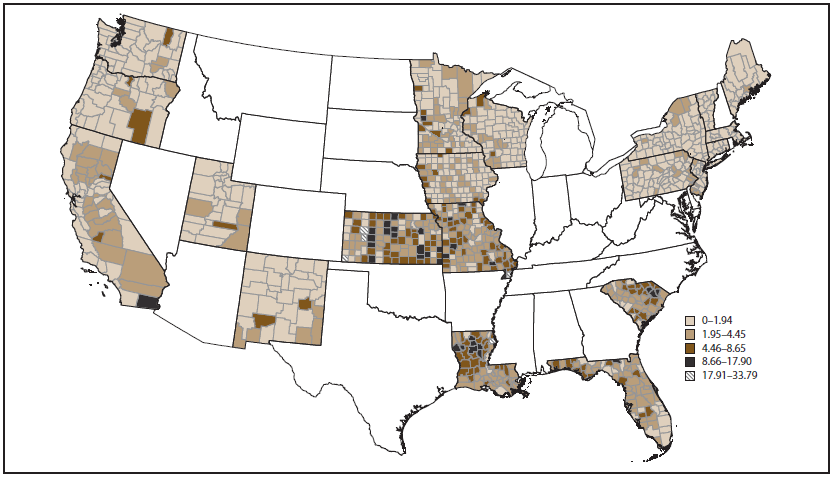
Alternate Text: The figure shows a map of the United States indicating the average age-adjusted rate of heat stress illness hospitalizations per 100,000 population, by county, for 20 states that participated in the Environmental Public Health Tracking Network during 2001-2010.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.
 ShareCompartir
ShareCompartir


